|
One of the most common questions I am asked during a wellness visit (routine physical) is "when should I get a colonoscopy?" . I was not asked this question as often 10 years ago or even 5 years ago, but there has finally been an increased awareness among the general population with colorectal cancer. As a former med/surg nurse, I took care of countless patients after their colonoscopy or even their colon resection for colon cancer. I helped care for their fresh colostomy site and stumbled to find the "right" words to give them comfort. I have one patient etched in my heart who lost his battle to CRC (colorectal cancer) at age 27. I was only 23 or 24 myself at that time. His young wife and 2 year old son stayed with him as much as they could. He had a suprapubic catheter (one that came out of his abdomen directly from his bladder to drain his urine) because the cancer had eaten through his entire pelvic cavity. I cried on my way home every time I took care of him. But I wanted to take care of him. I wanted him to see someone close to his age. Someone that didn't pity him like a child "poor dear" and all the other patronizing words I heard some of our senior nurses mumble. He and I would talk about TV shows and popular songs, whatever we could that would help him feel a little more "normal." This post isn't about him, it's about all of my patients. That said, I couldn't write this post without mentioning him because his life mattered and my time with him touched me forever. I could not write this post without telling you about another dear friend who lost his 6-year battle with CRC in 2020 at the age of 44. Out of love for his family, I will leave his story at that but HE MATTERED and MATTERS and cancer statistics are NOT just numbers my friends! They are mothers, fathers, sisters, brothers, sons, daughters, friends, employees, bosses, lovers, neighbors, coworkers, and beyond. The next time you see a cancer statistic on the news, I hope you pause and remember reading this post. So the question remains: When should I get a colonoscopy? In the words of my beloved GI colleague, "45 is the new 50!". The earlier CRC is found, the better the 5-year survival rate. We can easily remove a 5mm or smaller polyp in the colon and prevent it from ever becoming a malignant tumor. Yes there are some other screening tests on the market that have their place and time, BUT nothing beats a visual inspection by a well-trained eye looking for colon cancer. Direct visualization - there is nothing better!
The prep is not always "a gallon of nasty stuff" anymore either. There are a variety of prep techniques, so please don't let a colonoscopy prep prevent you from possibly saving your own life. You are NOT awake during the procedure. I have had one and I can tell you with certainty that I do not remember any of it AND I had zero soreness after the procedure. It was honestly a much-needed fantastic nap and a day off work. I urge you to see your PCP for a colonoscopy referral from a GI specialist if you are 45 years old or older and have never had one. If you have certain risk factors or family history, you should have a colonoscopy before age 45. Your PCP should be able to guide you. Any bright red rectal bleeding or alternating constipation and diarrhea needs to be worked up by your medical team. Please do not hesitate to seek care for those issues! I hope this answers your questions about colonoscopy screening. If polyps are found on your colonoscopy, your GI provider may want to repeat your scope in 2 years, 3 years, or 5 years depending on they type of polyp (per pathology diagnosis). If your colonoscopy is clear and there is no family history of CRC (or other extenuating risk factors), you will probably receive a 10-year pass. Most insurance companies pay very well for colonoscopy screening, BUT most insurances have a certain deductible each year that enrollees must meet, so do not be surprised when the procedure is not 100% free like your mammogram or pap smear was. Do not let cost stop you, though! It is well worth your insurance deductible. You can always call ahead to find out what your out-of-pocket expense will be, and most healthcare facilities offer payment arrangements. Please comment below if you have any other specific questions.
0 Comments
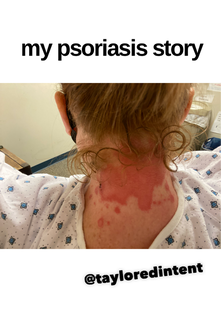
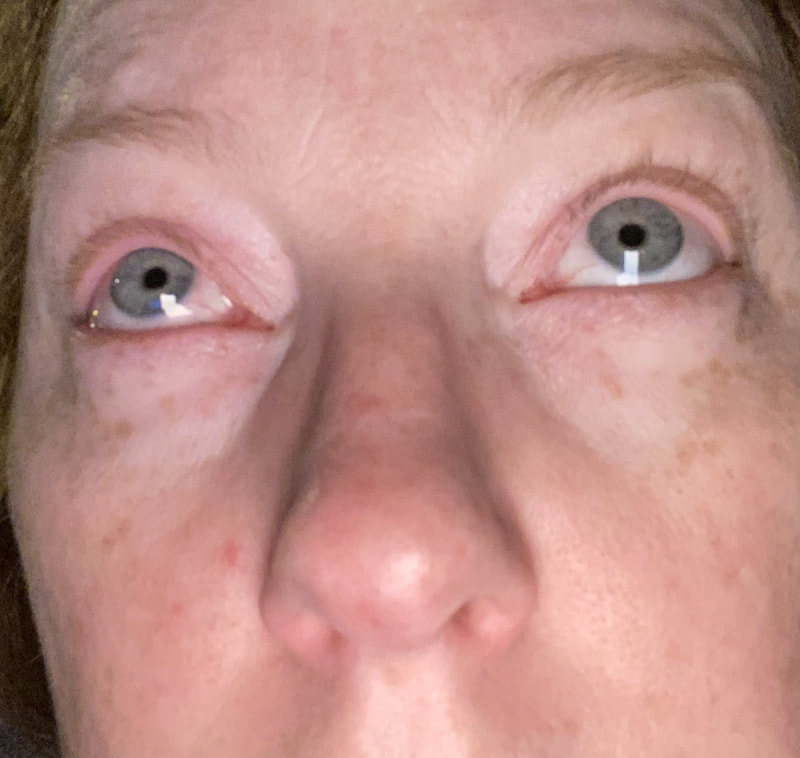
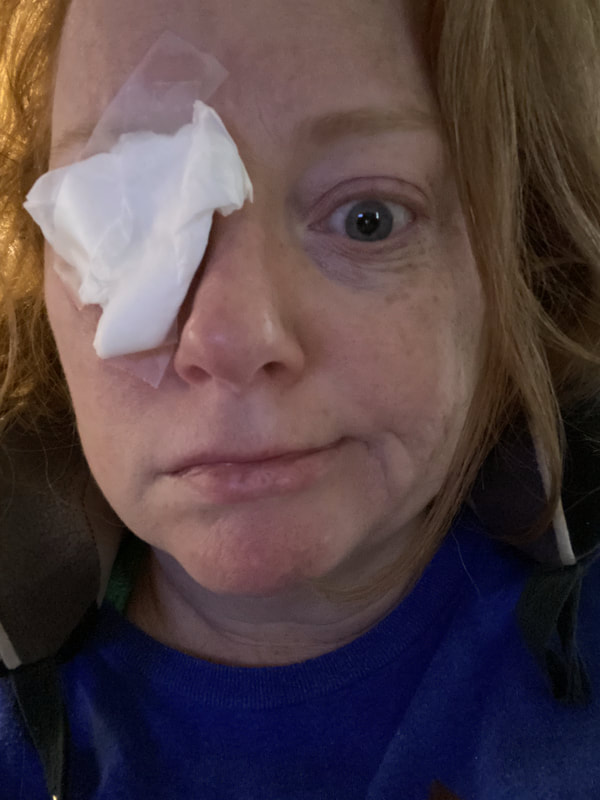
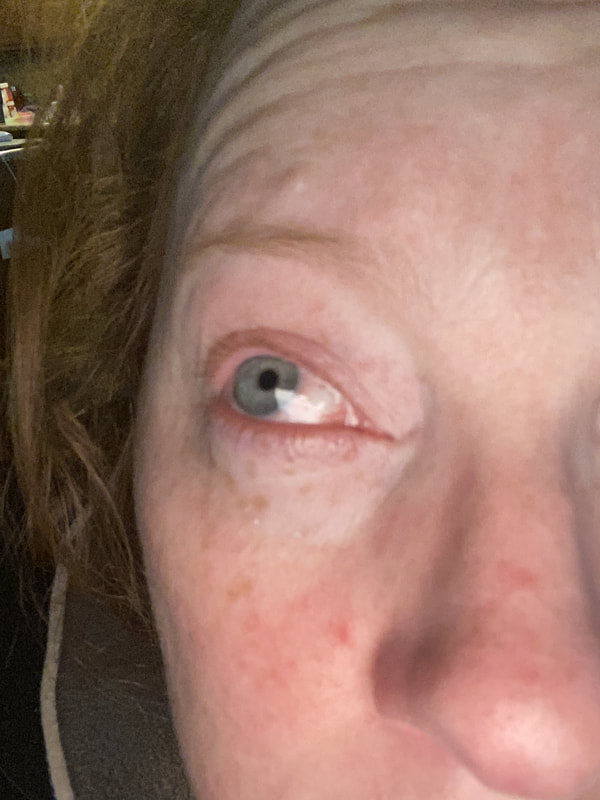
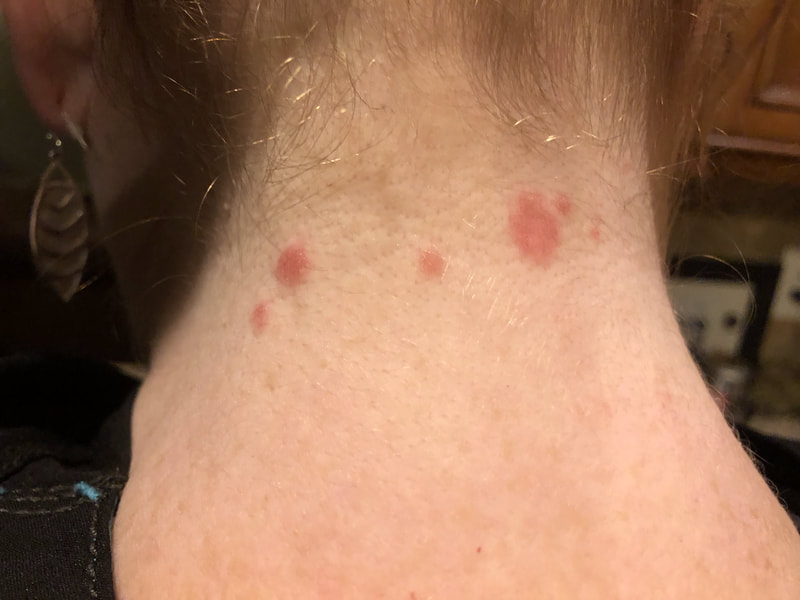
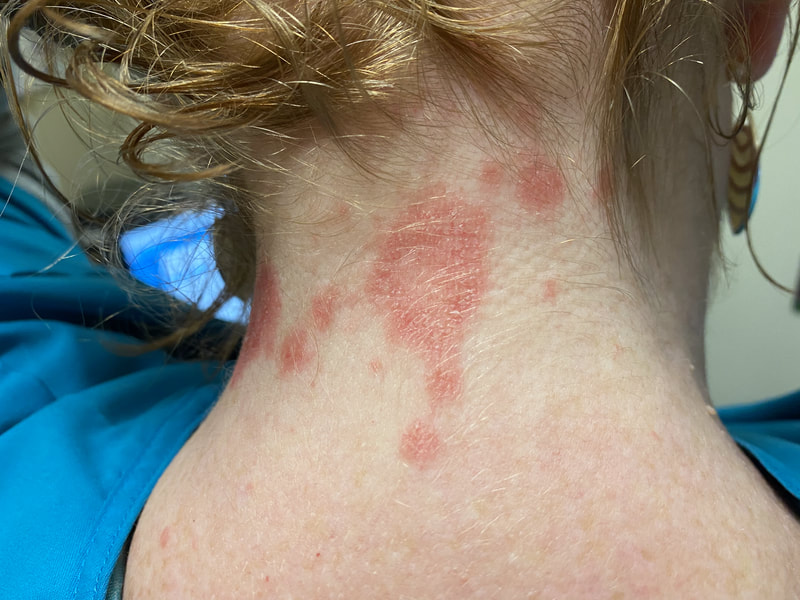
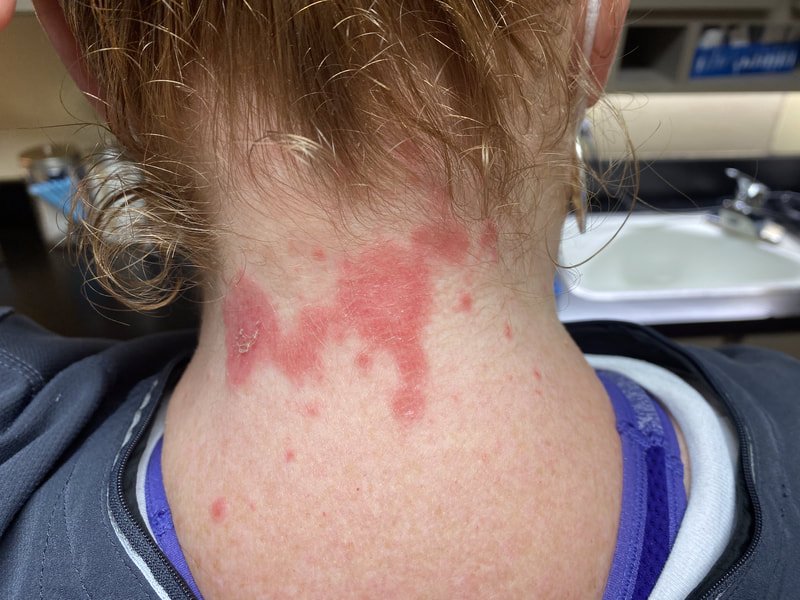
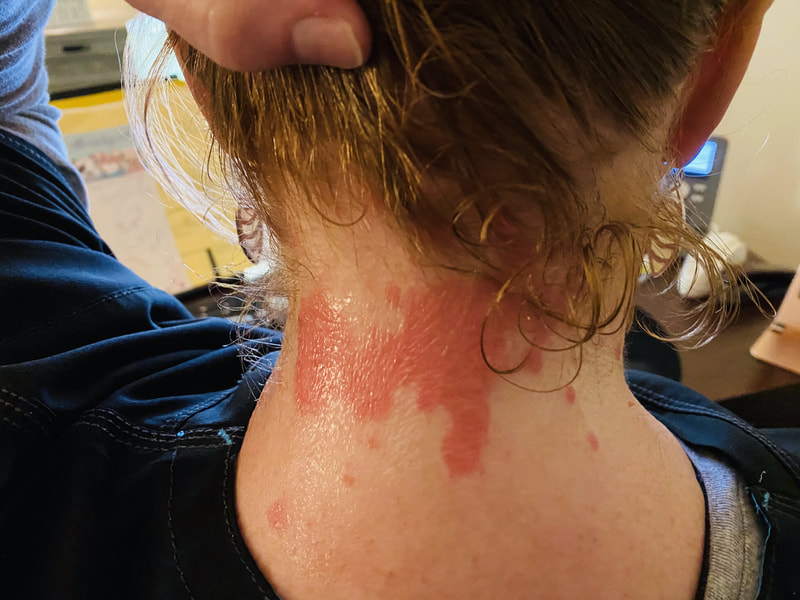
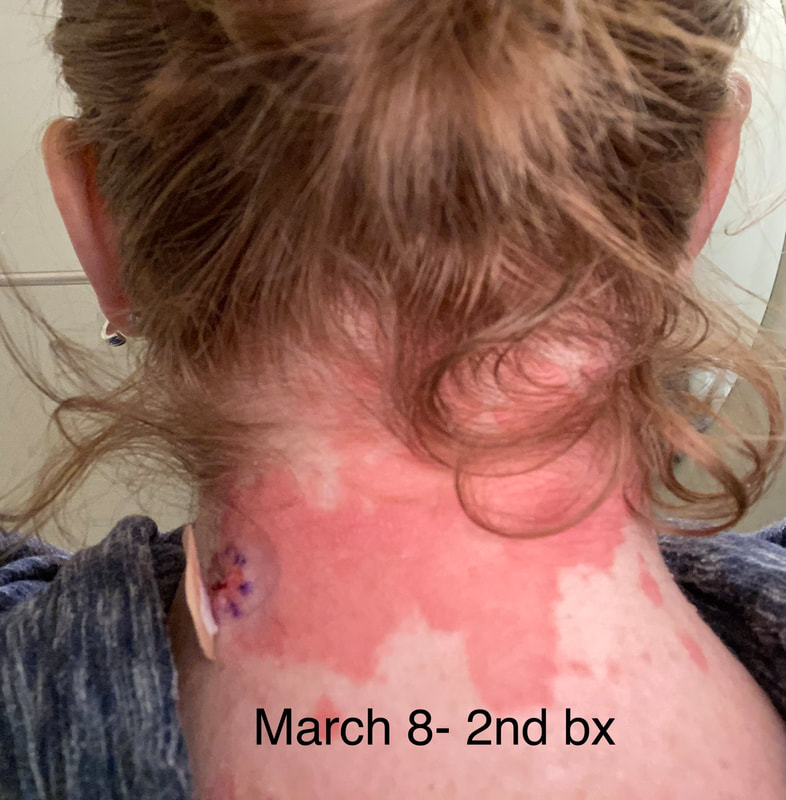
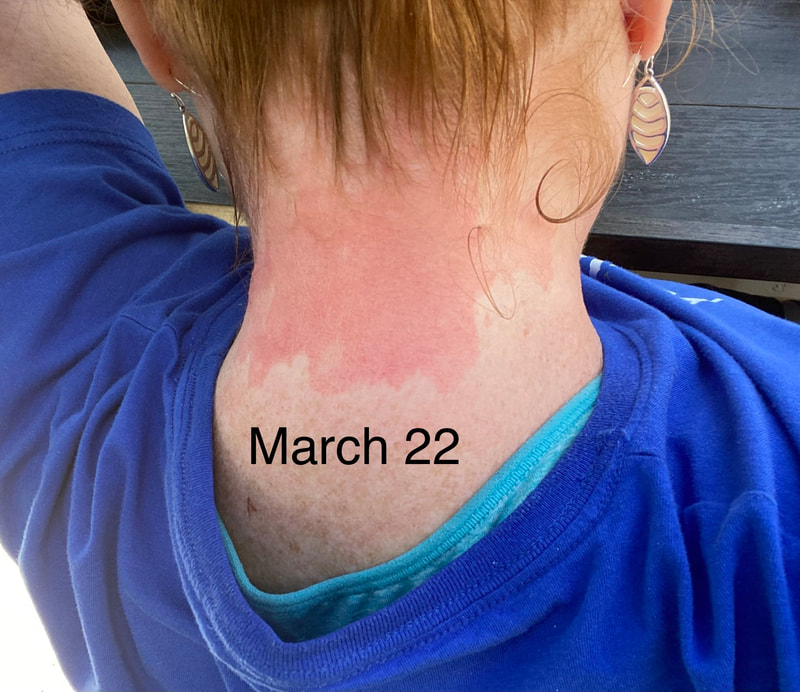
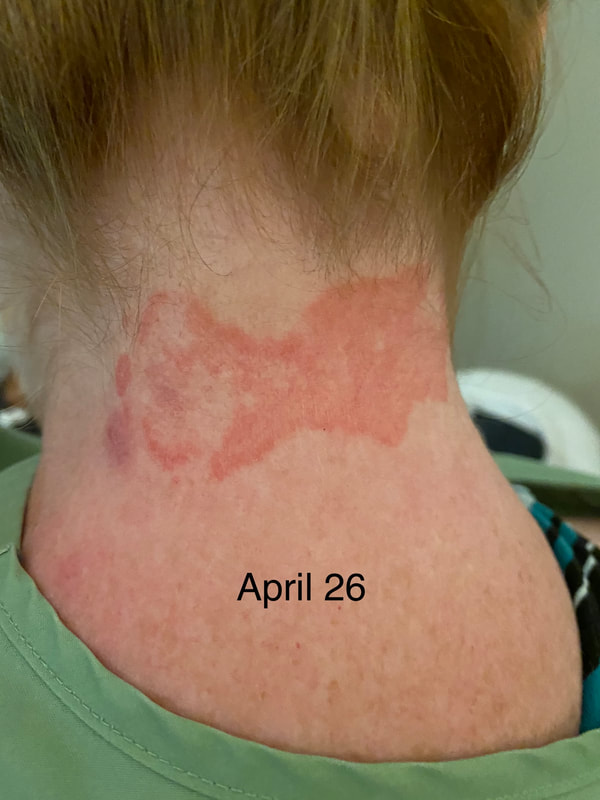
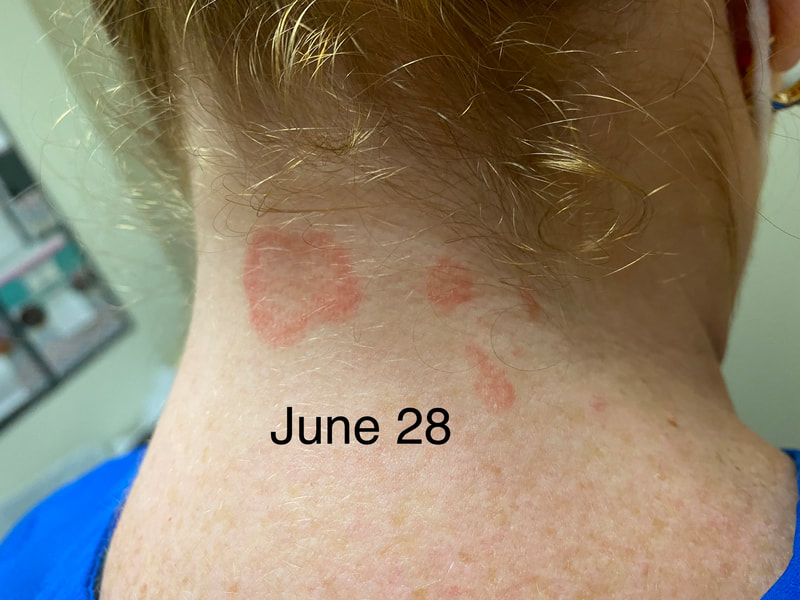
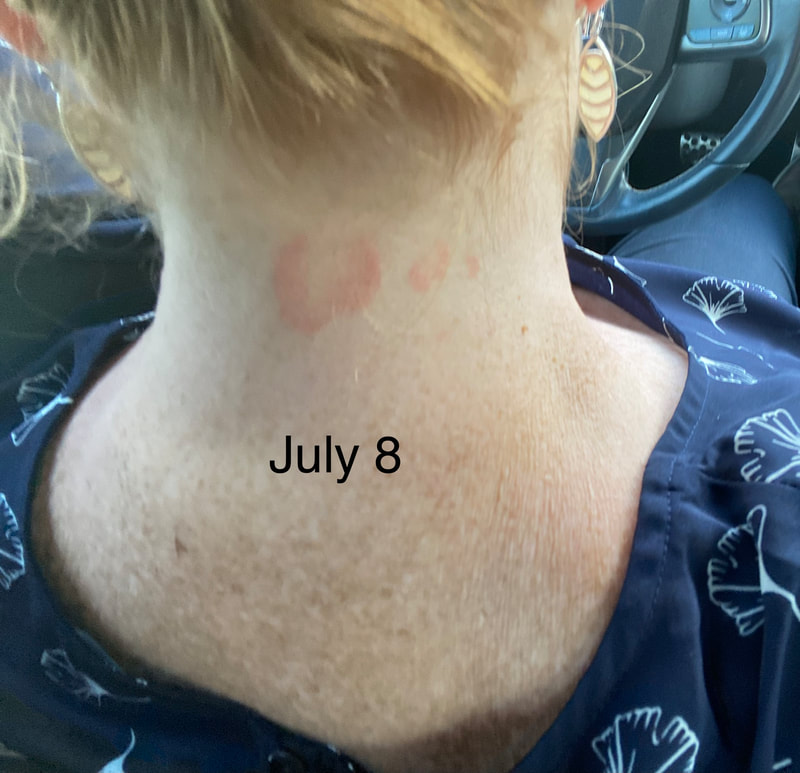
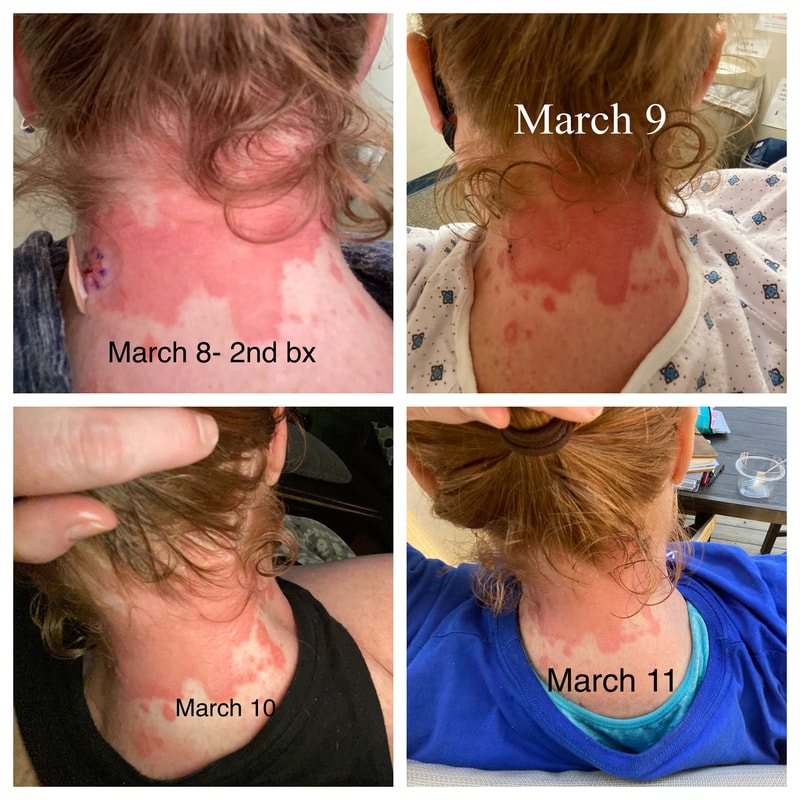
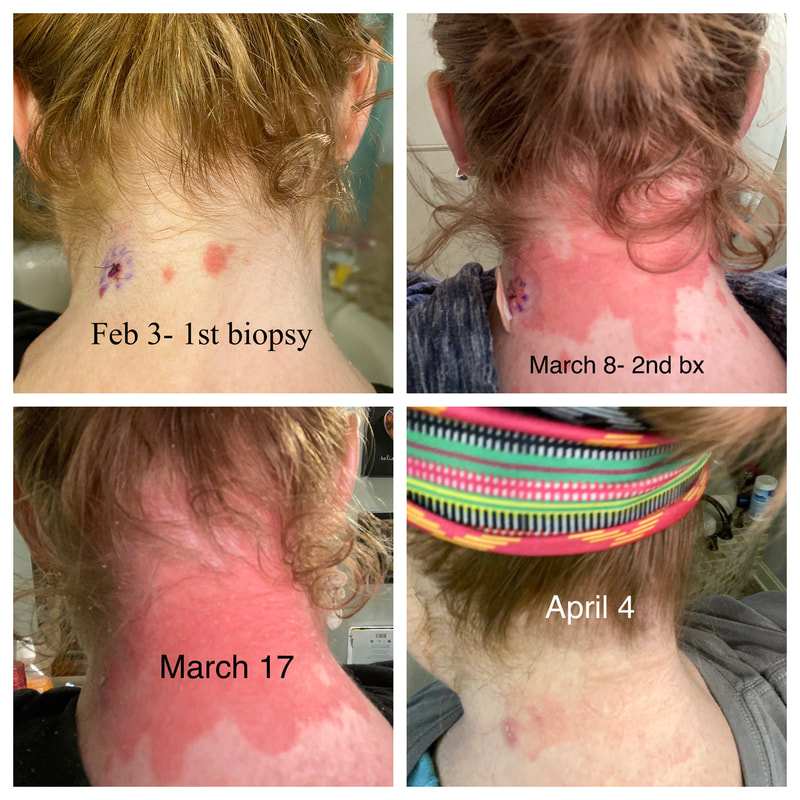
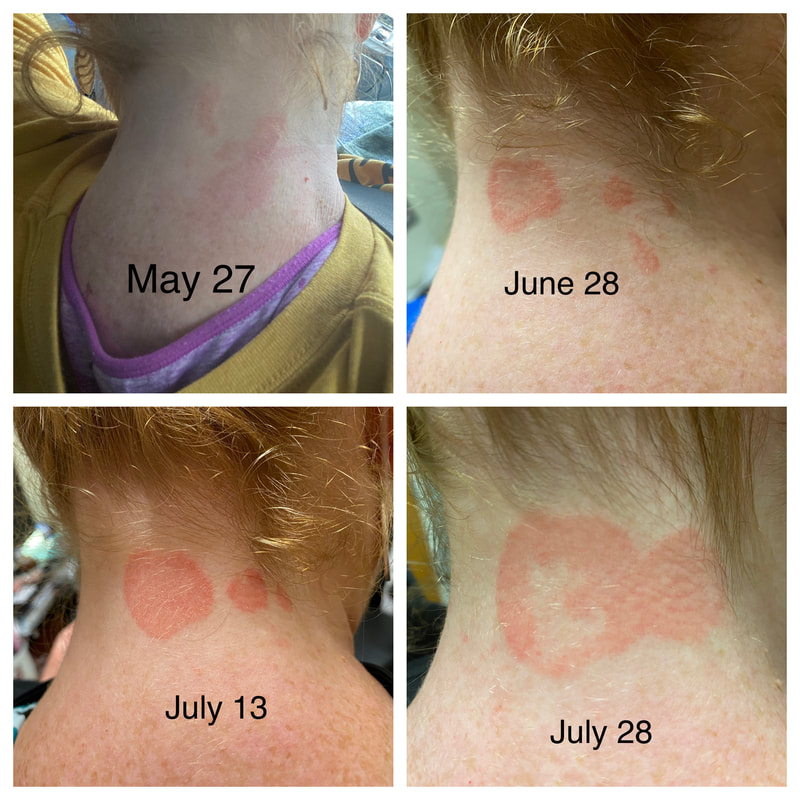
Jan 30, 2021- Feb 3, 2021 Red, painful eyes start with painful vision and light sensitivity (UVEITIS). Feb 3, 2020-Feb 8, 2020 Tiny dots of a rash begin on my neck- they don't itch, burn, or hurt at this point. I call my dermatologist to schedule a biopsy, assuming this must be related to my sarcoidosis. Feb 3-March 8, 2021 Rash kept getting bigger and more painful. Not responding to topical Rx creams. Went for 2nd biopsy on March 8th, the day I started my 30-day medical leave. Focused on walking, sleeping, hydrating, and eating clean. Also journaling and resting. March 8-April 8, 2021 Off work. Tried the AIP Diet. No gluten, no dairy, no sugar. Derm and Rheum also put heads together to double my Methotrexate dose. The diet was difficult but my joints and skin "felt" better even though my skin still needed lots of help! April 8- August 8, 2021 Back at work. Still working covid. Boys off for the summer during some of that time. Started Humira in May 2021 and stopped Methotrexate. Skin would wax and wane, but I would say it eventually cleared by early to mid-August. Joints feel much better on Humira. Energy level too. September 2021 Had my 2nd episode of uveitis. That responded quickly to Prednisone eye drops. Skin pretty clear, but under more stress with some work and family stuff. Delta variant of covid is ravaging my patient population and friends. Evidence of proteinuria again so will follow-up with my nephrologist (that's more sarc-related, less psoriasis-related). Still on Humira. Echo and PFT's slightly worse than last year, but lung & spleen CT's show that the Humira is controlling my sarcoidosis. March 2022 I have had at least 2 more episodes of uveitis since the last update. Skin stays mostly clear with the occasional flare in the anterior portion (front) of my neck. I wrote this piece for all of my fellow Psoriasis Warriors who are walking this painful, lonely road. It is SO HARD. One can think they are not a vain person, but when your LARGEST ORGAN (your skin) is literally on fire with inflammation, it's hard to "hide" from vanity, comparison, self-loathing, and frustration. If you love someone with psoriasis, please share this with them and with others who love them. I hope it brings someone comfort to know they are not alone and that there are those people who will love us no matter what. I just had a funny thought as I sipped my coffee. I wish I had read this article 19 years ago in my first few weeks of NP school. I wonder if I would have kept going to class? Probably... knowing me. I'm always trying to prove somebody wrong. Alright, alright, I'm about to let you all in on a BIG secret! Those who love me, and especially those who live with me know all of these truths, but I bet many of you are about to lose all your enamor for your health care provider. I am going to tell you about the daily life of a family nurse practitioner working in primary care. In essence, my day can be broken down into a few "sessions" or time periods.
Let me laugh with another sip of coffee real quick before I proceed.
Going back to my original "dreams" of working as an NP, did any of it come true?
Check out these posts from my fellow Hope*Writers for our monthly writing challenge. This month's theme was "daily": Oh, I Try by Jessica Weaver www.rootedunrooted.com/blog/oh-i-try Kids Sleep Meditation: 6 Daily Practice Dos and Don’ts by Ashley Olivine louvaria.com/kids-sleep-meditation/ Lessons from Daily Bread by Dianne Vielhuber simplewordsoffaith.com/2021/09/01/lessons-from-daily-bread/ Daily Conversations with God by Sharla Hallett www.sharlahallett.com/daily-conversations-with-god/ Pros:
Cons:
I have worked as a family nurse practitioner since 2004. As with any career in medicine, I have had peaks and valleys. Burnout and frustration countered by personal reward and gratitude. Humility for sure. In nursing school, I liked every rotation. I wanted to do "all of it." My faculty advised me to go into med-surg. I guess my love for "all of it" carried into my choice to primarily stay in family practice. I have done some moonlighting in GI and Pediatrics. GI was interesting, a challenge, and a break from a full family practice panel of patients. Pediatrics was fun, repetitive, and just a different pace. I think any career in medicine comes down to a few things:
In the words of Thoreau "It's not what you look at that matters. It's what you see."
How to have an effective office visit with your provider: There are some tried and true ways to have a productive, meaningful visit with your medical provider. As a patient with a chronic illness AND a family nurse practitioner, I have the inside track.
If you need more frequent office visits, ask for them. Your provider is PAID to see you. Your insurance is billed for those visits where as most providers do not bill for phone calls or portal messages. If you end up needing them before your designated 3 or 6 month follow-up and you have more than 1-2 simple questions, PLEASE schedule an office visit. As a provider with complicated patients of my own, I would much rather have that patient in the office with me to have a discussion than to do multiple back-and-forths over the portal. It’s better patient care. AND my time is used wisely in my employer’s mindset. Medicine is a business. Although so many of us really do care!!! Healing people is wonderful. It’s challenging and rewarding and exhausting and sad and scary and exciting and mundane. It’s refills and phone calls and charts and labs. It’s insurance authorizations and having the same conversations with the same patients over and over and over again.
But it’s also seeing progress and growth and determination. It’s witnessing families come together and sometimes fall apart. It’s being a steady presence in the lives of what starts as strangers and ends as friends. Can we be friends? Am I your friend? I like you. I’m cheering for you. I want you to do well! I think of you and I pray for you. I laugh and I cry with you. I love seeing your pictures of your babies and your successes. My heart hurts when you hurt. Where are the boundaries? I don’t want you to have my cell number, but I want you to tell me when you need me. How does that work? What are the rules and who makes them? I don’t want to think of you as just a name or a number. I am invested in you and you in me. Working in a small town feels like home. It’s likely that I know your mom, your neighbor, your hairdresser, and your child’s teacher. I wouldn’t want it any other way. At the end of our time together, I want you to smile when you think of me. I will always smile when I think of you. Even if you didn’t heed my advice. Even if you missed too many appointments. Especially then, because you made me work harder. I want you to know I looked forward to walking in your room and seeing you just as you are, whatever you were going through. I am thankful you put your trust in me. I know you made me laugh at least once. I saw you, all of you. I think you saw me too and I’m okay with that. |
Proudly powered by Weebly