|
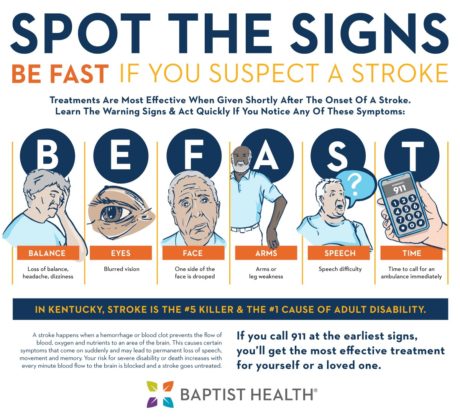
In my 24 years of nursing / NP work, I have seen countless cardiac events either in action or the ramifications of such events. On a personal note, three of my four grandparents had strokes. I lost my paternal grandfather when I was only 4 and he was 55 due to a massive stroke. My paternal grandmother had stents in cardiac and non-cardiac arteries as well as "open heart surgery" CABG (coronary artery bypass graft). I have been affected by heart disease on a personal and a professional level, and I want to help patients understand the true risk of death and debility associated with cardiac events. Here are the top 10 reasons I refer patients to the cardiologist:
Let's talk a little more about each of these 10 conditions and how a patient may actually present to my office with these symptoms.
I have had patients in their thirties suffer from strokes and heart attacks. I have seen heart failure, cardiac arrhythmias, and high blood pressure in patients from childhood, young adulthood, and beyond. I doubt there is anyone in America who does not personally know someone who has been affected by heart disease. In honor of America's Go Red for Women Month (every February), I encourage you to schedule your wellness exam with your primary care provider and to start paying more attention to your heart rate, blood pressure, water intake, weight changes, and dietary choices. Your heart matters to me! Godspeed.
0 Comments
I see it every year. It starts around the first week of November and it lasts through the middle of January. The holiday blues. As I’ve gotten older, I’ve actually slowed down enough to think about trends in my practice. Sure there is an actual diagnosis of seasonal affective disorder, but this is different. This is deeper. This is hard. And here’s how I see it every day for two months straight in my exam rooms: Me: Hey Mrs. Jones - it is so good to see you. I know we had to zoom for our last visit. What’s new in your life? Are you ready for Christmas? Do you have to cook for Thanksgiving? Are y’all going anywhere? Mrs Jones: oh you know, I will be cooking for the family for Thanksgiving. And the children and the grandchildren may stop by for Christmas. No... I don’t go anywhere. I’m ready as I’ll ever be. Blank stare. Obvious reflection. Anyway how are your boys? Are they ready for Christmas? Do you have to cook for Thanksgiving? Me: oh yes I will be making my Mammaw’s dressing, sweet potato casserole from an old Birmingham recipe from one of my mother’s friend’s mothers, my layered salad that a nurse I used to work with taught me how to make. Gosh that was over 25 years ago now. Blank stare. Obvious reflection. Daddy will fry the turkey and my husband will fix the ham and a peanut butter pie. Mama will make the deviled eggs and the Waldorf salad. I will make my mother-in-law‘s corn bean casserole and some homemade mashed potatoes. Of course we will have rolls and cranberry sauce. Another blank stare. I haven’t seen my mother-in-law in over five years. The boys? Oh yes, they are more than ready for Christmas. We got them a matchbox Advent calendar they can’t wait to get started on. They’re growing up so fast. Blank stare. Obvious reflection. The oldest will be home from the Air Force. He and his girlfriend will be together the whole time I’m sure. I smile. But I’m nearly in tears. What is going on? And we sit for a moment. Two women born of different decades and sometimes different skin colors who have lived two very different lives at the outsider’s glance, but are so alike on the inside that it’s haunting. Her daughter is sitting beside her. They look and act so much alike it makes me smile from the inside out. I’m sure that’s what people say when they see me with my mother. I don’t have a daughter. Will my boys take care of me? Alright, get it together Amy. We finish out our actual medical visit and say our go-to goodbyes: Happy Holidays. Y’all be safe. Call me if you need me. And now, after ALL these years, I often hear “you know I love you.” And I believe it’s true. It’s not forced. It’s been earned. Is it against the rules? No, not my rules it’s not. Truth be told, I love her too. Maybe because I see myself in her and I’m cheering for myself in my old age. I’m giving myself a head start and saving myself a seat. I’ve practiced in Kentucky and in Georgia. I worked in a nursing home for six years and then made rounds as a nurse practitioner in that very same nursing home. I’m an old soul myself so I think I draw my elderly patients in and they stick. I stick to them too, and I think they know it. I’ve had so many Mrs. Jones over my 17 years. I’ve had Mr. Jones and Little Johnny Jones or Little Sally Jones as well, but I am so connected to Mrs. Jones that I can almost finish her sentence. Now I’m driving home and this 2 Lane Highway surrounded by trees and cows and horses makes me feel like I could be in any of the four states I’ve lived. It’s familiar and so are these thoughts. I’m a little girl in my childhood home with my brother and my parents and we just came home from candlelight Christmas Eve service and mama made lasagna. I haven’t really been hurt yet. I don’t know what it feels like to love somebody besides my family. I feel safe and secure and like I can do anything in this world. How did Mrs. Jones feel at this age? How did you feel at 10 years old? Now I’m driving home from Tuscaloosa with Delta Zeta on my back windshield. My finals are over. I get to see my boyfriend. I’m taking pre-med classes as well as a full nursing load, but I’ve been hurt by now. I’ve been disappointed and lied to by some people I trusted. But it’s the holidays you see, and I still feel like I’ve got a handle on things. I wonder what Mrs. Jones was doing at 20 years old? Had you been hurt by then? Oh wow. I didn’t really see this coming. Or did I? I’m sitting alone in my first marital home. Half my furniture is gone. Someone I love deeply told me I don't really need a Christmas tree this year because "it's just you." Am I not enough for a tree? Who am I by myself anyway? I’m driving to Georgia for Christmas. I don’t think I’ve ever been this sad in my life. I wonder what Mrs. Jones was doing when she was 30 years old? Was her heart broken like mine? Was yours? Gather around now. It’s time to eat. My baby boy is four years old and can’t seem to stop smiling. God gave him to me for sure. The first one I carried is six and almost as smart as I am. The one I didn’t carry but I’ve fed and loved now for seven years is sitting right next to me. Is he thinking about his mama? Will he ever see her again? Tiny pieces of my heart crumble for him. I just started taking prednisone for an incurable autoimmune disease I had to look up on the Internet. Lord have mercy and I really do mean "please Lord have some mercy." I’m only about 3 1/2 weeks into a lifelong diagnosis and I don’t know what the future holds. I’m scared. I’m sad. Merry Christmas y’all. It’s the holidays, right? I wonder how old Mrs. Jones was when she first questioned her mortality? How old were you? Were you 40 years old like me with a child in pre-K, one in first grade, and one silently falling apart right in front of you? You see that’s what the holiday blues are. They are every heartbreak and broken promise. They are all the fears and all the lost relationships. They are that empty seat at the table. The phone that barely rings. They are the one that got away and the one that stayed too long. They are your mother, your father, and your children. They are every husband you’ve ever had. How can they not be? We can’t erase our memories. I don’t have a cure for the holiday blues. I think they’re part of life. Mrs. Jones might tell me they get better with each decade or she might tell me they grow and take up more space than we should allow. I’m scared to ask her. None of us even talk about it really. We just say Merry Christmas, Happy Holidays, y’all be safe. So this is my letter to you at age 45. Some heartaches of mine have healed and some are still there. I don’t think we should only remember the good times because that’s not what made us. It’s certainly not what made me today sitting right here baring my soul and giving you the permission to bare yours. Acknowledge the things that built you. Godspeed. This goes out to every Mrs. Jones that has ever allowed me to know her. She is me and I am her. And I thank God for that. A popular book in the field of marriage and relationships is Gary Chapman's The Five Love Languages. In his book, Dr. Chapman discusses the five core languages used to give and receive love. Knowing your love language and that of your partner is quite beneficial as you navigate various scenarios and frustrations throughout your relationship. I will link the quiz below. The 5 Love Languages according to Dr. Chapman are:
Originally written in 2004, the book has now sold over 6 million copies. I read it when it was originally released, and I read it again when I remarried. I knew the importance of speaking the same love language (or at least being aware of my partner's love language) . I think it is helpful to know your close friends' love language and the language of your children or other close family members. If you are not familiar with the concept, I will use this brief example: Amy (acts of service, physical touch): " I am so tired. Ugghh I have so much to do. I don't know how I'm going to get it all done." Husband thinking to himself (words of affirmation, quality time): Amy is so tired. She should go to bed. Maybe if I keep encouraging her to go to bed, she will. Amy thinking to herself: If he would fold this laundry, then maybe I could go to bed. But instead he's just telling me I should go to bed. Husband thinking to himself: Why is she folding that laundry when she is so tired? If I offer to fold the laundry, she may lash out at me since she's so tired, and (needing words of affirmation) that would ruin the night, so I will just stay with her (quality time) and gently encourage her to go to bed. Amy fuming at this point (acts of service, physical touch): If he's not going to fold the laundry, he could at least rub my back. Then maybe I could relax enough to go to bed. But husband doesn't rub my back because he wants the words of affirmation and reassurance to do so and the spiral continues. Neither spouse did anything WRONG, but remembering each other's love language might have made for a much more pleasant evening. Pleasant evenings bleed into smooth mornings and so forth. This example is just one of many. It can apply to family, friends, coworkers. You may be trying to show appreciation with a gift or money but they WANT / NEED to hear you say why you appreciate them. They may be doing all the little chores and acts of service to get your attention, but you WANT / NEED them to stop running around and spend the afternoon with you without any distractions. It really is fascinating once you know the love language of your partner or best friends. You can spend an entire afternoon dissecting why one situation went south based on love language miscommunication alone. But back to PHYSICAL TOUCH, I think this love language is often overlooked and misunderstood. For obvious reasons, it's viewed with caution, and while that is good... it is also robbing us of a basic human need. With the surge of technology and virtual everything, many of us go days or weeks without touching another human, particularly these last 2 years. Throughout my career, I have used touch as a means to reassure and connect with my patients. Since I received touch as a child and infant in a safe, healthy environment, I have been able to give touch easily. I know that is not true for everyone I encounter, and I acknowledge that. Here are some ways I have used touch in my practice:
Here are some ways I have used touch in my home with my children:
My challenge to you, wherever you are, however old you are, whatever childhood you had, whatever love language you prefer, however many times you've been hurt, is to THINK about physical touch in the setting of a newborn baby. I have linked an article below touting the science behind touch and neurological growth and development. If you're old enough to find this article, then you have been a child yourself. You may have children or be involved in a child's life. We all know that a crying baby or toddler is often soothed by the touch of a loved one or caregiver. Animals are the same way. I dare say, adults are ALSO the same way. If you love someone (your child, your partner, your mother, your close friend), touch them. HUG them. Incorporate safe and healthy touch into your daily routine. We have grown generations of adults now who are not used to being touched. Those untouched adults are now having more untouched children. Those untouched children are looking for affection in ways that a simple "cuddle session" (what we call it at our house) may have averted. It saddens me when I shake a teenager's limp and nervous hand or attempt an appropriate side-hug with someone and am greeted with surfboard-stiff awkwardness. I see the physical and emotional effects of the untouched in my office each week, and it breaks my heart. Pat Harris was my first grade teacher. She had a Hug-Me-Spot right by the door to her classroom. No student could enter her room in the morning or leave her room in the afternoon without hugging Miss Harris on the Hug-Me-Spot. This world needs a Hug-Me-Spot. This world needs an army of Miss Harrises. The rules and restrictions have created a generation of kids that don't know what touch is actually appropriate, and adults that are too glued to their phones to use their hands to rub their child's back or snuggle on the couch. These touch-starved kids marry each other and are LONELY and starving for affection that was never modeled for them. And here we are. I challenge you to touch someone today. And tomorrow. And the next day. Hug. Cuddle. Kiss your partner. Squeeze your child. Hold hands. Make touch a part of your day every day. We may really change the world. 🌎 Let's try it. ☀️ Godspeed.
Before deciding if you love me or hate me, let's look at each of these in a little more detail. If you are reading this and you don't work in healthcare, I encourage you to close your eyes. Imagine driving to work where patients are very sick and you are responsible for their health. Imagine being extremely exhausted - mentally, physically, and emotionally. Imagine having the same conversations day in and day out. Imagine wearing a mask and face shield all day every day AND if you work in certain healthcare settings, full plastic gowns (sweaty and HOT) with even more restrictive masks (n95). Think about having heart-wrenching conversations about death and dying with families and patients that you have come to love over many years. Consider praying on your drive in and your drive home because you've worked in healthcare since you were 19 years old, but you've never seen anything as dark and dangerous, cold and pointless, savage and destructive as THIS. Imagine that you, like everyone else, have also been unable to see loved ones, travel, send your kids to school without a mask, and that you- like everyone else- have your own political and religious beliefs but you cannot mention those since ALL eyes and ears are on you. Now imagine doing that every single day for 20 months in a row.
I usually wrap up my posts with some heart-swelling, tear-jerking, or funny concluding thoughts. I try to connect us as humans, mothers, fathers, daughters, sons, sisters, brothers, neighbors, and friends. I find a way to touch you, soften you, move you even if it’s only for a moment. I don’t know how to do that with this post. I’m tired. I’m sad. I’m frustrated. I’m still hopeful. I still believe. I guess I will end by asking all of us to consider the division we have all felt over the past 2 years. Consider the lost lives and energy we have all spent to prove we are right. And hug your family. Hug your loved ones. And look your “enemy” in the eye before you judge their choices. We really are all the same. Imperfect. Scared. And trying to stay alive. 🌎 When a patient presents with hair loss, I obtain a thorough history:
I then perform a thorough physical exam and order the following tests:
That may not “answer” your question but I hope it helps you know what a clinician will be looking for with this presentation of hair loss. 🩺👩⚕️ Personally, I have dealt with hair loss from taking Methotrexate for my sarcoidosis.
It started coming out in clumps in the shower and then in my brush. I soon had very patchy areas of hair loss all over my scalp. My hairdresser advised me to stop applying heat to my hair when possible, to wash my hair less frequently, to avoid ponytail holders when possible, and to avoid any hair color or harsh chemicals. I usually got some blonde highlights in the spring put in my naturally red hair, but I went without those for 4 years while I was on Methotrexate. My rheumatologist increased my Folic Acid dose from 1 mg to 2 mg daily, and I ordered Biotin off Amazon Subscribe and Save. I took the Biotin daily to help with hair growth. I am finally off Methotrexate and on Humira and am seeing hair growth again. Losing my hair was very emotional for me. My bright red hair has defined me for so long. I now knew what all of my patients struggling with hair loss from chemo or other medical reasons were feeling, and boy was it a wake up call. My heart goes out to anyone struggling with hair loss. Much love to you and I hope this helps. I was surprised 🧐 when the vaccine came out for frontline HCW (healthcare workers) in December 2020 and the general public started claiming it caused sterility. Let’s use common sense. 🧠 It takes 1–24 months 📆 to conceive before most providers start to investigate infertility. It takes 40 weeks to carry a baby 🍼 to term. Let’s average conception time to 12 months and add the gestation time of 9 months🤰 to = 21 months. Covid REALLY started to hit the US hard about 18–19 months ago. The vaccine was available to some of us 9–10 months ago but MOST of the women of childbearing age could not receive it until 5 months ago. How can anyone claim infertility at this point in time? 🤔 I never say never because I am constantly learning in medicine. Every day I see something I never thought I would witness. I have had pregnant women🤰contract Covid and pregnant women🤰receive the Covid vaccine. I have also seen pregnant unvaccinated women with Covid whose babies had to be delivered while mom was on the ventilator. My community just lost a 28 year-old mother of 3 who never got to know her newborn. 🥲 The American College of Obstetrics & Gynecology and the Society for Maternal Fetal Medicine issued a joint statement encouraging the vaccine for all pregnant women🤰 in July 2021. I recognize that I have the benefit of being "done" having my babies as I navigate this pandemic. That fact is NOT lost on me. I know young adults are faced with a very hard decision with such a new vaccine and their entire lives in front of them. Early in the pandemic, I even advised some of my young, healthy patients to wait until we had more long-term data... that I saw no serious health risk if they were to contract covid. 2021 changed that. I have had YOUNG, healthy patients on the ventilator and near death. I still believe it is a personal decision, but please be sure you are getting your information from reputable sources and people you trust. Much love...
Bonus question: what can I do to help? I feel so helpless!
***as always, consult your PCP for your healthcare. I’m trying to raise awareness. Let’s not bicker and judge over vaccine status. Let’s educate ourselves and let’s come together to get out of this public health crisis!!!***
This is a great question and one I have seen asked many times on many platforms.
I have 2 autoimmune diseases (sarcoidosis and psoriasis) and take Humira. Prior to Humira, I was on Methotrexate. I took my first Pfizer dose in December 2020, second in January 2021, and I received my third in Aug 2021 since I qualify for the third dose now. I read the pfizer trial and the data is phenomenal. I had zero side effects all 3x other than a sore arm. That is my patient experience. As a primary care provider, I manage a panel of about 1800–2k patients. I’ve had ZERO deaths or serious side effects from the vaccine in my panel. I have had 2 deaths (age 78 with lung disease, age 49 and healthy), over 225 infections, countless hospitalizations - some requiring ventilation, and I am seeing long-term effects from COVID: stroke, pulmonary embolus, neuropathy, still haven’t regained taste / smell, palpitations & arrhythmias, chronic fatigue, chronic brain fog, and lung damage. I think the vaccine is being “pushed” because I know I can’t keep up with the volume of sick patients I’ve seen in the past 18 months. I know every ICU in my state is now on diversion. I know we as healthcare workers are leaving the field due to burnout. I’ve never seen anything like it and I’ve been a nurse 23 years, an NP for 17 of those. ***Always consult your PCP for your healthcare. I trust and believe in the vaccine, but I do not think it should be mandatory. Let us not bicker over vaccine choices, but let us come together and try to get out of this public health crisis!*** What can I do at home for Covid? 1. Zoom with your provider 2. Walk around as much as you can- covid causes blood clots 3. Lay on your belly when you’re resting, not necessarily when asleep. We are proning Covid patients (placing them on their belly) even when they are on the ventilator to help move mucus / fluid and drain the lungs. 4. Hot steamy showers. Even if you don’t feel good enough to shower, sit in your smallest bathroom with the steam running to help open up the lungs. If you feel lightheaded though, stop. 5. Hydrate hydrate hydrate - covid is an inflammatory virus and hydration is key! 6. Monitor your pulse and oxygen levels as I mentioned yesterday. 7. What has fallen out of favor / lacked statistical backup and/or caused harm: ivermectin, oral steroids prior to hospitalization, hydroxychloroquine (Plaquenil), unnecessary antibiotics 8. Mucinex, zinc, Vit C, Vit D, Singulair (it’s Rx though) are all in the grey zone- I don’t think they’ll hurt you but they may not keep you out of the hospital. 9. Finish out your quarantine please and thank you. 10. Chest percussion- look it up on YouTube How do I know if it’s Delta? 1. Big testing centers are batch testing swabs for variants and extrapolating that data to identify geographic variant trends. Your local urgentcare is not. 2. Whatever the variant, we treat based on symptom severity and delta may look good on you and horrible on Sally. Alpha (the original variant) may have put me in the hospital but barely slowed Steve down. 3. I equate it to flu A and B which are always swabbed and tested together each year. Every year I hear “oh Flu B is way worse than A. I’m so sorry you have B.” Etc etc etc when patients’ flu courses can vary regardless of the strain. 4. Anecdotally, my zoom covid visits with this wave seem different than in 2020. Less fevers. Less complaints of crippling headaches. Less loss of taste and smell. More dizziness & confusion (likely from low oxygen levels). Similar diarrhea complaints. Worse shortness of breath and chest tightness. Way more trips to the hospital and ICU. . My only vent-survivor told me all of a sudden they just Could Not Breathe. I should add this person is under 40 years old and is (or was) healthy. 5. Speaking of strains, did you know the Gardasil vaccine protects against 9 strains of HPV? Did you know Prevnar13 protects against (you guessed it) 13 strains of pneumonia? Strains have been around forever as have vaccines yet sudden interest persists. Just educating- no judgment on vaccine choices. I’m too tired. How many times can a child under age 12 have Covid? Will they develop immunity? Great question. I’ve seen twice so far and I expect more. Their bodies should be developing antibodies but no children have volunteered for my quantitative antibody study yet. Stay tuned. How soon should I get my vaccine after I have Covid? I’m recommending one month not 90 days IF you’re truly feeling better. Ask your PCP as they know your health situation. If I’m + today, symptoms resolve in 2 weeks, and then I’m + in 4 weeks, is it a reinfection or residual positive from original infection? I would ask if you ever had a negative test. If you did, maybe it is a re-infection but if you did not, I know we saw some folks stay + for 6 weeks or more in 2020. ***as always, consult your PCP for your healthcare. I’m trying to raise awareness. Let’s not bicker and judge over vaccine status. Let’s educate ourselves and let’s come together to get out of this public health crisis!!!***
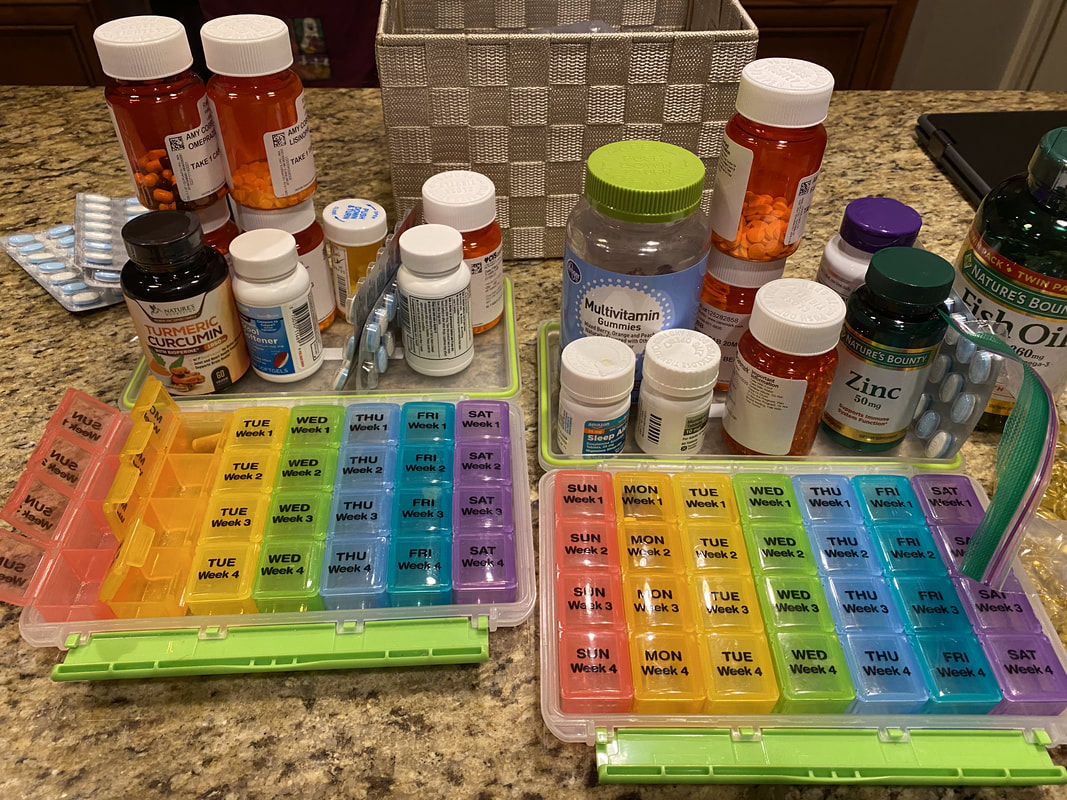
Taking multiple medications multiple times per day can be overwhelming at best. Remembering to take them, remembering to refill them with the pharmacy, remembering to contact the provider if you run low, and remembering to purchase or pick them up can be stressful, time-consuming, and somewhat depressing. I hate filling my 2 pill boxes each month (one for morning, one for evening). It is a reminder that I am living with a chronic illness and that my body has "failed me." My rheumatologist told me 5 years ago at the onset of my sarcoidosis diagnosis, "Amy, my goal is for us to get your treatment regimen in line to the point that you only think about having an illness when you see me every few months and when you take your medication. Otherwise, I want you to feel so good that you don't even think about it." I did not know then how important those words would be to me five years later. I have FINALLY recruited my husband to help me fill these PITA boxes (they are- I spill meds every month and lose count without fail). Now we turn on Ted Lasso or Bloodline and he fills one while I fill the other. It is depressing to accept that my body depends on the very THING I shell out every single day in my profession. I can truly empathize with my patients who say "but I don't want to be reliant on a pill." A few times I have shown them a picture of my med boxes, and sometimes it has provided comfort. One patient asked "oh my goodness- what is wrong with you?" so I decided I might share a little less. Vulnerability is hard. My best advice is to have a system for managing your medications if you have a chronic illness.
Throughout my career, I have had to deliver hard news to my patients. I have had to deliver even worse news to their families. It is the LEAST favorite part of my job, but I have found some comfort knowing I am delivering the news with compassion and empathy. I usually know the patient and family very well, and I think that means a lot. These suggestions may be helpful when faced with a difficult diagnosis.
Let's look at each suggestion in detail:
I am in a unique position in that I have both delivered and received hard news. At the age of 40, when my youngest son was 4, I was told I probably have lymphoma AND multiple sclerosis over the phone by a nurse. I was told to get an appointment with an oncologist and a neurologist as soon as possible. Many blood tests, imaging tests, and biopsies later, I was finally told that "you don't have cancer! And I don't think you have MS but I'm not sure. What you do have is a lifelong incurable autoimmune disease that can attack any organ and can be difficult to treat. And by the way, nobody has really heard of it and even us doctors have to google it when we see it on a chart."
So maybe those weren't his exact words, but it was close. And there will be a lot more to that story to come in my posts. I wish someone had used tip #3 with me when delivering my news. Here are 10 easy ways to support someone with a chronic illness:
I have been living with a chronic illness for 5 years now. My family and friends have been a huge source of support. Even as they've tried to love me, I've witnessed their looks of "what can I do?" or "what should I say?". Most chronic illnesses are unique and involve multiple appointments with various specialists, countless medications, and years of simply managing one's health. These concrete examples can really help your loved one and make them feel important.
How to have an effective office visit with your provider: There are some tried and true ways to have a productive, meaningful visit with your medical provider. As a patient with a chronic illness AND a family nurse practitioner, I have the inside track.
If you need more frequent office visits, ask for them. Your provider is PAID to see you. Your insurance is billed for those visits where as most providers do not bill for phone calls or portal messages. If you end up needing them before your designated 3 or 6 month follow-up and you have more than 1-2 simple questions, PLEASE schedule an office visit. As a provider with complicated patients of my own, I would much rather have that patient in the office with me to have a discussion than to do multiple back-and-forths over the portal. It’s better patient care. AND my time is used wisely in my employer’s mindset. Medicine is a business. Although so many of us really do care!!!  What do we say when we don't know what to say? We have all been there. Someone dies unexpectedly. Someone receives a terrible diagnosis. A divorce comes out of nowhere. A tragic accident. Our partner says something cruel or doesn't meet our emotional needs. A friend is struggling with infertility or has a miscarriage. Our friend is venting about a difficult situation. Here are some tips for what to say and what not to say: Do / say this:
Don't do / say this:
CHECK OUT THE BOOK "I HEAR YOU" BY MICHAEL SORENSON FOR AN IN-DEPTH DISCUSSION ON ACTIVE AND EFFECTIVE LISTENING. WORTH THE READ!
Healing people is wonderful. It’s challenging and rewarding and exhausting and sad and scary and exciting and mundane. It’s refills and phone calls and charts and labs. It’s insurance authorizations and having the same conversations with the same patients over and over and over again.
But it’s also seeing progress and growth and determination. It’s witnessing families come together and sometimes fall apart. It’s being a steady presence in the lives of what starts as strangers and ends as friends. Can we be friends? Am I your friend? I like you. I’m cheering for you. I want you to do well! I think of you and I pray for you. I laugh and I cry with you. I love seeing your pictures of your babies and your successes. My heart hurts when you hurt. Where are the boundaries? I don’t want you to have my cell number, but I want you to tell me when you need me. How does that work? What are the rules and who makes them? I don’t want to think of you as just a name or a number. I am invested in you and you in me. Working in a small town feels like home. It’s likely that I know your mom, your neighbor, your hairdresser, and your child’s teacher. I wouldn’t want it any other way. At the end of our time together, I want you to smile when you think of me. I will always smile when I think of you. Even if you didn’t heed my advice. Even if you missed too many appointments. Especially then, because you made me work harder. I want you to know I looked forward to walking in your room and seeing you just as you are, whatever you were going through. I am thankful you put your trust in me. I know you made me laugh at least once. I saw you, all of you. I think you saw me too and I’m okay with that. |
Proudly powered by Weebly