|
If you have a pet of any kind, you know the joy that pets bring into our lives. While they do come with a certain level of commitment and work, they offer benefits that far outweigh what they require of us. Now that I am six years into my primary chronic illness, sarcoidosis, I feel like I can discuss pet therapy with conviction. Prior to becoming "sick," I always had a pet - from childhood on. It wasn't really until I became ill, however, that I realized what my dogs had done for my mental health. My physical health has also improved thanks to being a pet-owner. Here are 10 ways owning a pet can help you with your chronic illness:
Charlie the Dachshund is always there for me. He will wait on me wherever I go and follow me no matter what. He needs my help to get his food, water, and to let him outside. It feels good to be needed by someone or something that doesn't really expect much in return, ESPECIALLY with a chronic illness. I can be sick, tired, or both in front of him and not feel self-conscious. I can tell him all my thoughts and fears, and he won't judge me. I can even moan out loud in pain or cry at my medical misfortune and he doesn't flinch. Instead, he meets me with loving kindness and is a steady force of calm in my daily life.
0 Comments
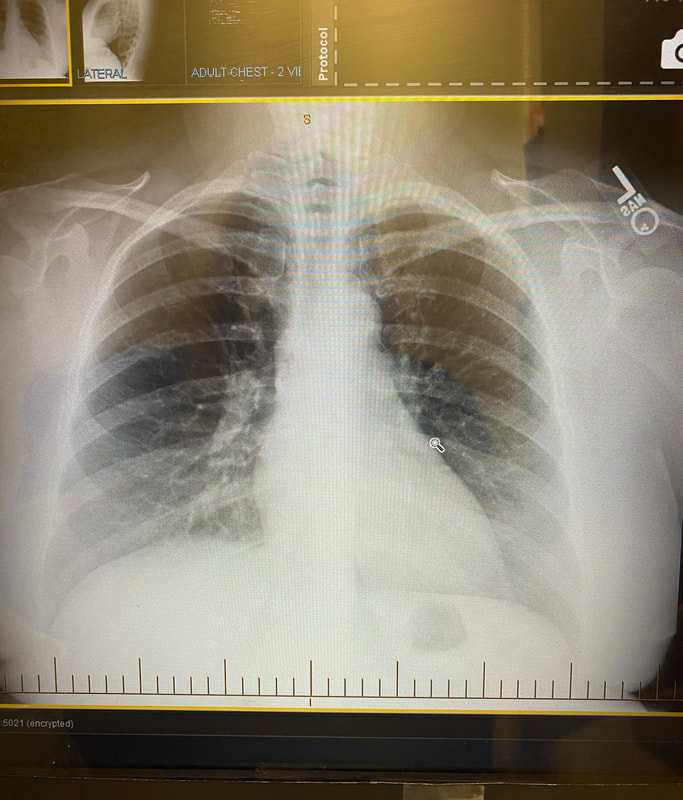
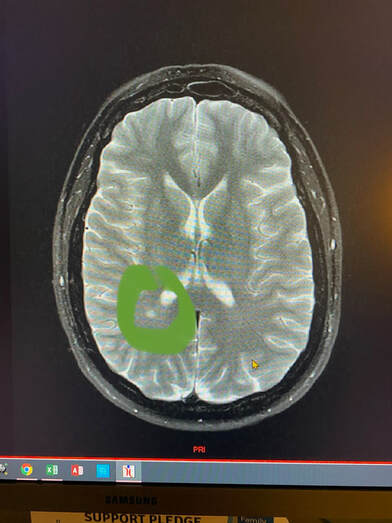
In 2016, at the age of 40, I received a sarcoidosis diagnosis that rocked my entire world. My kids were 4, 6, and 14 at the time. I was at the pinnacle of my NP career, and I was coming off a 2 year "break" from full-time work. From 2014-2016 I was working 2 or 3 days a week and was able to spend more time with my family. I was also able to go to the gym regularly and prepare healthy meals. I felt like my health was also better than it had been in the past 7 years. My sarcoidosis symptoms started abruptly in September and were very noticeable. I would walk to my car that was parked on a hill after work and be extremely short of breath (think huffing and puffing as if I had just sprinted 100 yards). I would go to the gym and feel completely wiped out after 20 minutes of my workout when normally my full hour workout left me energized and not depleted. I would walk out of an exam room and forget the name of a medication or stop mid-sentence when trying to give my nurse a verbal order. I also felt very dizzy and lightheaded and was not sure what was causing all of my symptoms. I decided to go see my colleagues in cardiology once I realized my blood pressure was dropping. My blood pressure was dropping as low as 80s/50s. I was also having numbness and tingling in both arms and hands and my hands were turning blue. I thought there had to be some type of blockage or blood flow issue. Ultrasound evaluation of my carotid arteries and upper extremities were normal. EKG, basic labs, and chest x-ray were normal. My echocardiogram (heart ultrasound) was the first test that came back abnormal. It showed an elevated pressure reading between my heart and lungs (pulmonary hypertension). My providers were not really sure what would be causing that because I was "so healthy." I plugged along from early September to late September before seeking a second opinion. My symptoms were progressing and persistent, and I knew something was not right with my body. My fatigue was worsening to the point I would count down the hours until I could get into bed. My shortness of breath was limiting my daily activities and I was beginning to cough every time I ate or talked for more than a few minutes. I also had an episode while driving where the left side of my face went numb and my breathing became very shallow and irregular. That sent me straight to my second opinion! That second provider ordered a chest CT and a brain MRI which were performed on a Thursday morning. That following Monday in early October, I was at work for a 12-hour day. I received a phone call mid-morning from a nurse in my second opinion provider's office. The nurse said "you have brain lesions and you need to see a neurologist to rule out MS (multiple sclerosis). You also have enlarged lymph nodes throughout your chest and you need to see an oncologist to rule out lymphoma." As you can imagine, I was in shock and called my manager to tell her I needed to leave for the day and to go speak to my husband and my parents. Did I mention my youngest child was 4 years old? Fast forward to a bronchoscopy mid-October with lymph node and lung needle biopsy as well as a trip to a neurologist which resulted in EEG and extensive lab testing. My neurologist ordered more MRIs and tried to ease my fears of MS (though he could not totally rule MS out). My pulmonologist was unable to get a conclusive diagnosis from the bronchoscopy and recommended a mediastinoscopy which would involve drilling through my sternum (breastbone) to remove lymph node tissue for biopsy. I told him that I felt a large lymph node above my left clavicle and we opted to have that node excised for pathology instead of the mediastinoscopy. That left supraclavicular node excision was done the last week in November under general anesthesia at the hospital since it was so close to my carotid artery and jugular vein. That node biopsy was negative for lymphoma and positive for non-caseating granulomas (the definitive diagnosis for sarcoidosis). I was started on 60 mg of Prednisone per day that would be tapered over 6-12 months and referred to a rheumatologist.
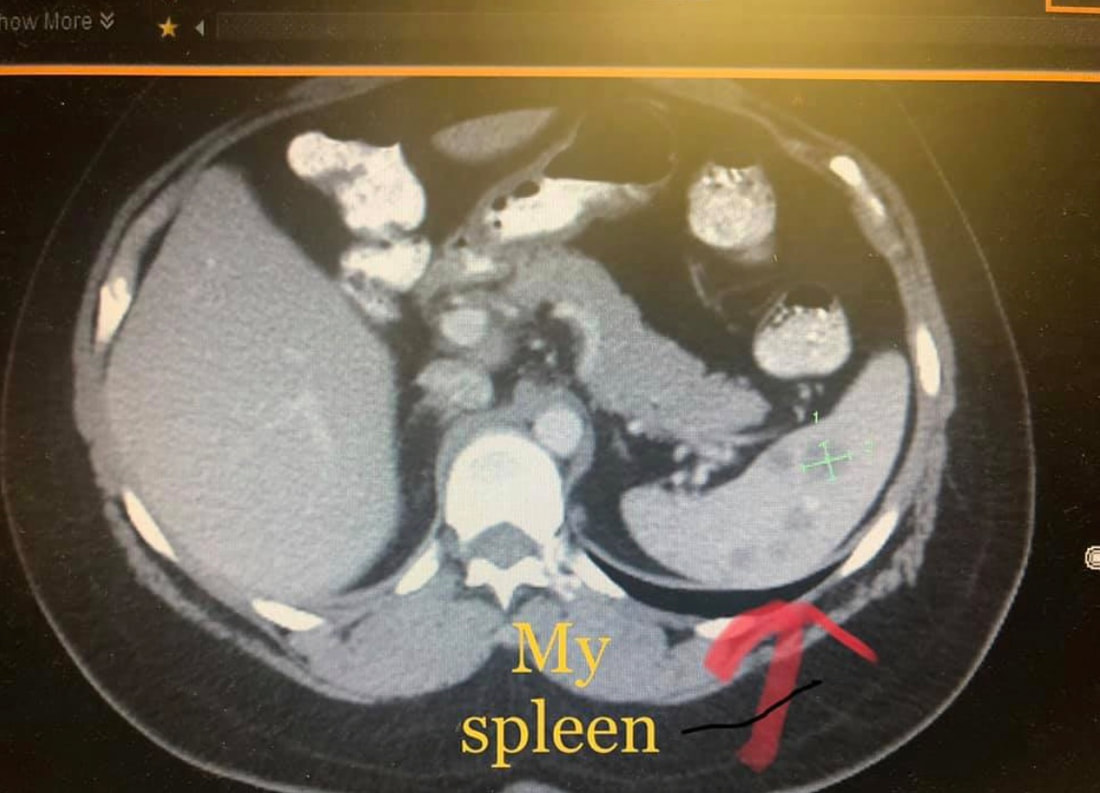
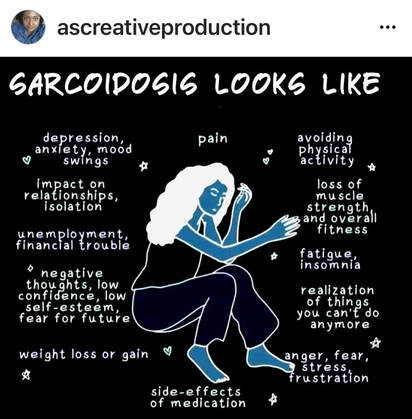
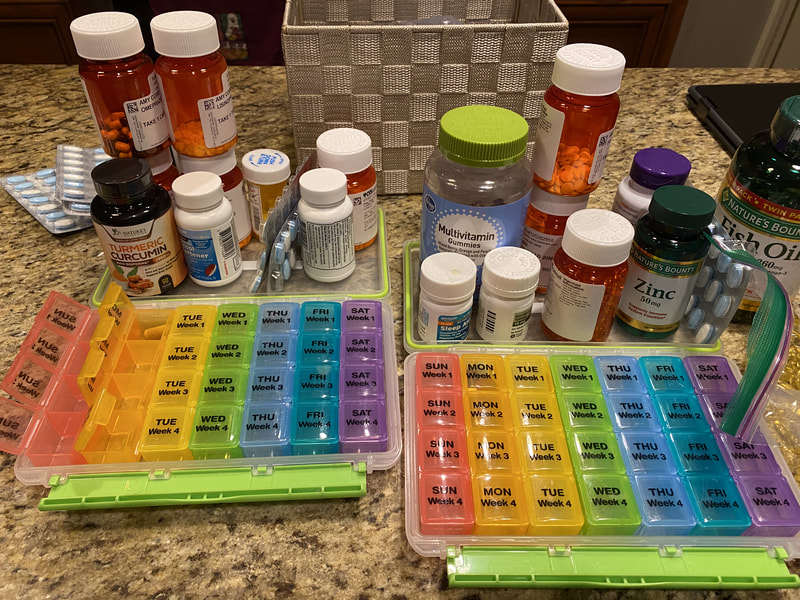
After starting high dose Prednisone in December of 2016, I was placed on weekly Methotrexate injections which (who knew at the time?) would last another 4 years. The only reason I stopped Methotrexate is because I later developed psoriasis (for that story, click here). I was finally able to wean off prednisone late May 2017 though the side effects lingered at least another 6 months. I plan to write an entire post on surviving long-term prednisone, but I will leave it at that for now. 2017 seemed somewhat stable throughout the end of that year, but the next 3-4 years had their own hiccups. Over those next 3-4 years I found out that the sarcoidosis was affecting my esophagus. 3 EGDs in 6 months and tons of other GI testing led to the conclusion that my esophagus has no peristalsis ("squeeze'). The only thing helping my food reach my stomach is gravity. This makes eating challenging, especially talking while eating (cough, choke). I also found out I had sarcoidosis spleen lesions, ocular involvement, and another fun lung condition called bronchiectasis. For the esophageal involvement, I take 2 pills per day for life. For the bronchiectasis, I take one pill twice a day for life. See how I organize my meds here. I have also been tested and monitored for small fiber neuropathy. The MS surveillance continues. My neuropathy is currently of unknown etiology, but my neurologist does think sarcoid plays a role. I was also sent to endocrinology at one point to check for adrenal insufficiency after steroids since my blood sugar and blood pressure still bottom out at times. Another hiccup involved an overnight hospital stay and a kidney biopsy (ouch by the way) after I noticed my urine was foamy like dishwashing liquid (that is abnormal and a sign of protein in your urine- tell your provider if you ever see this). I'm on another daily pill to help protect my kidneys for that confirmed renal sarcoidosis. Every year I see a rheumatologist, general cardiologist, pulmonary hypertension cardiologist, pulmonologist, gastroenterologist, neurologist, ophthalmologist, dermatologist, nephrologist, and my PCP and Gyn. I now see a counselor regularly to help me process all that I juggle. I have mandatory quarterly labs, an annual heart ultrasound, CT's and MRI's every year, breathing tests every year, and whatever else comes up. Gone are the days of a routine wellness visit or not meeting my deductible. Gone are the days of only taking a multivitamin. I sleep with oxygen mainly for the pulmonary hypertension, and I'm okay with that. It was my little secret until now. Right now, my sarcoidosis seems fairly well-controlled with Humira. When I met my rheumatologist in 2016, he told me he hoped he could get me into remission within 2 years. That was 5 and a half years ago. I haven't given up hope and I will continue to fight this fight as long as I can.💜 Below, I have included two great visual aids to raise awareness for our family and friends. The mental health effects of sarcoidosis are widespread and often overlooked by our clinicians. Sometimes just "being there" is all we need from our loved ones. 💜
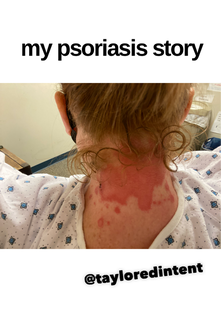
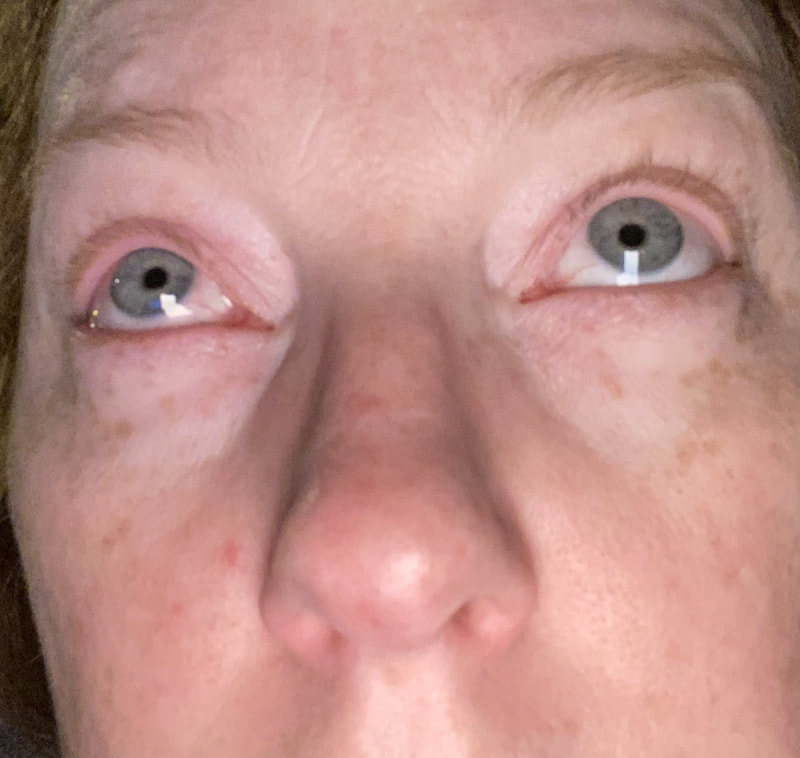
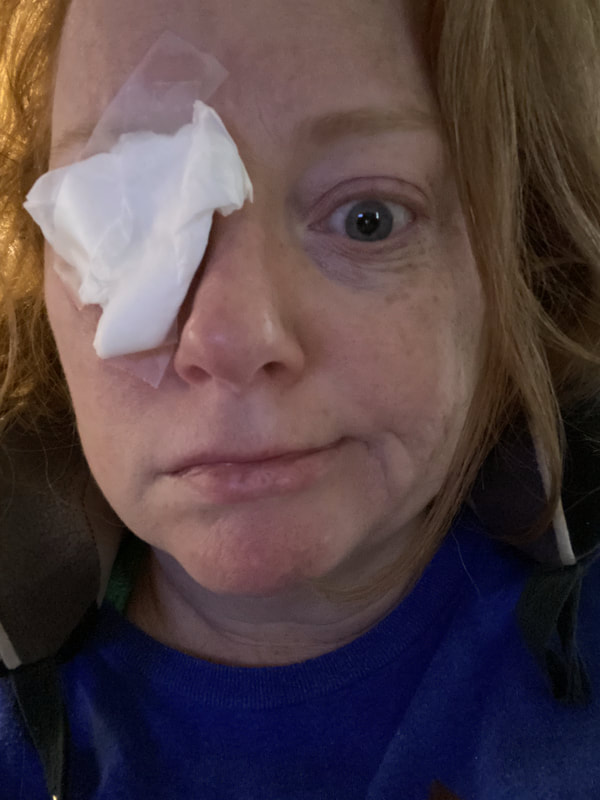
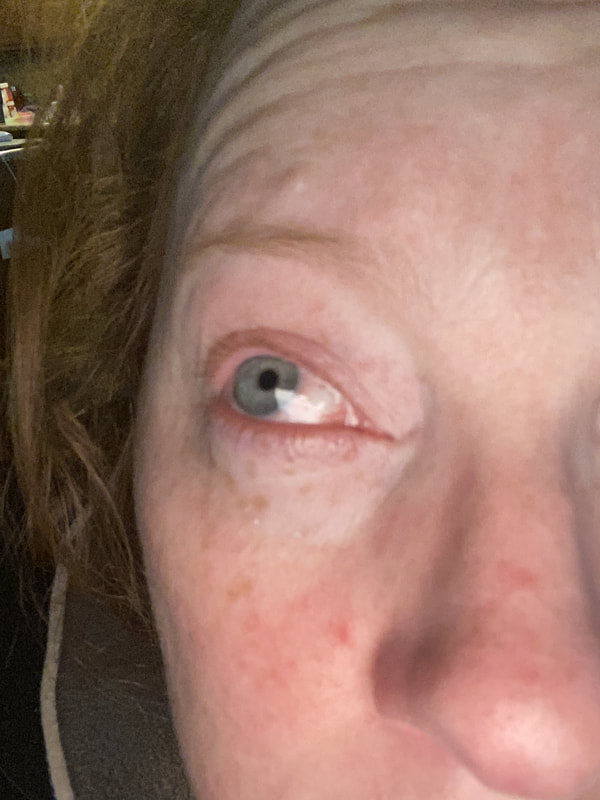
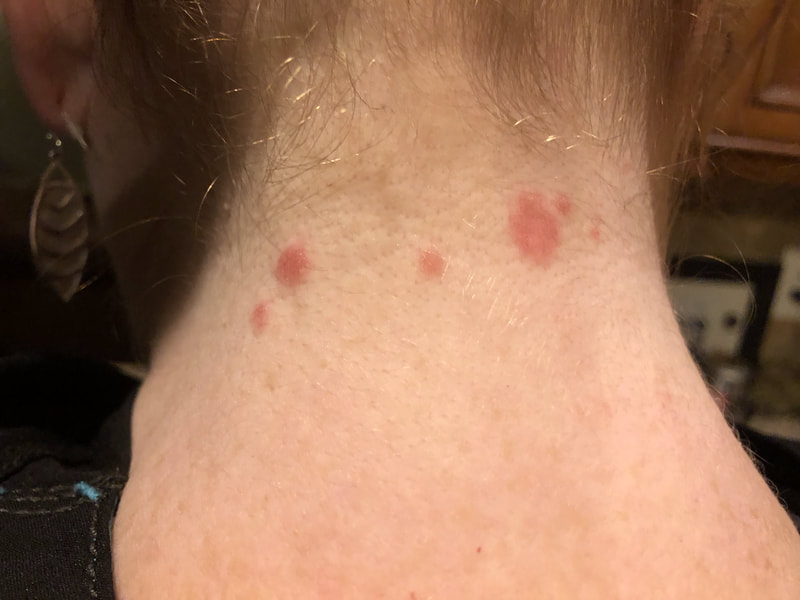
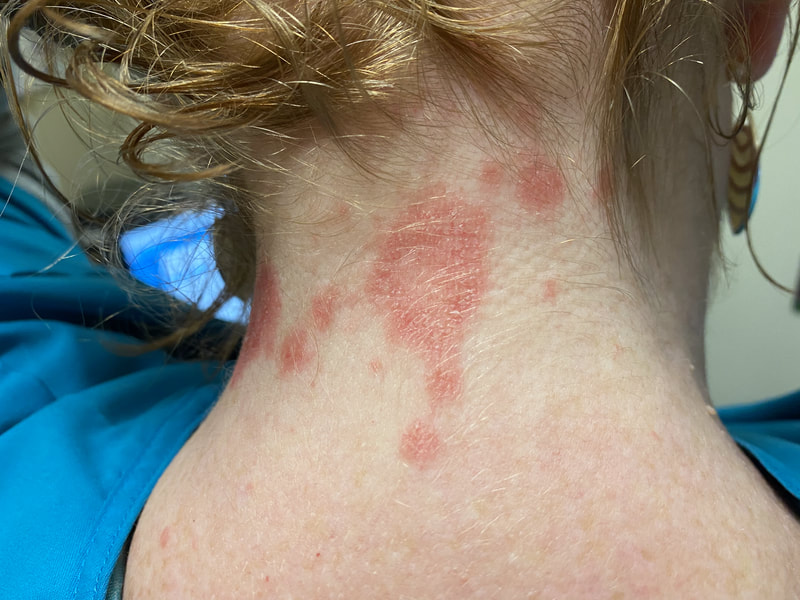
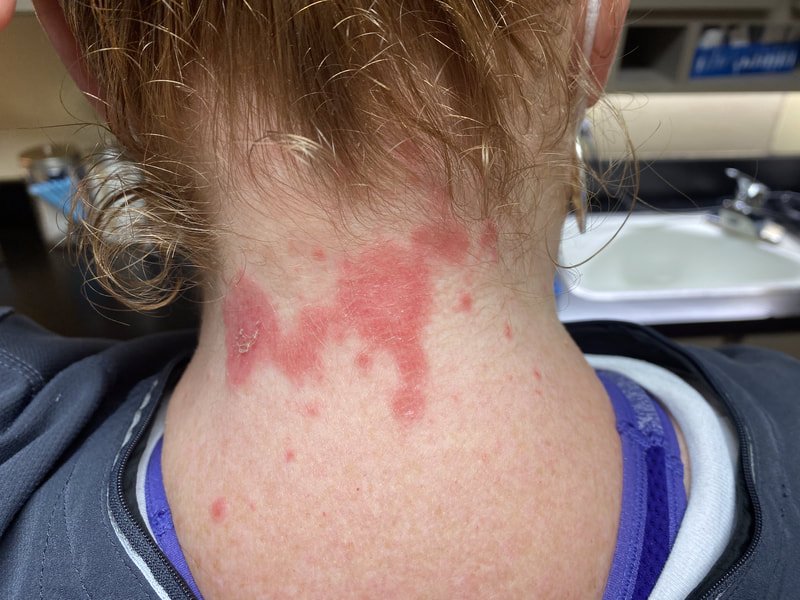
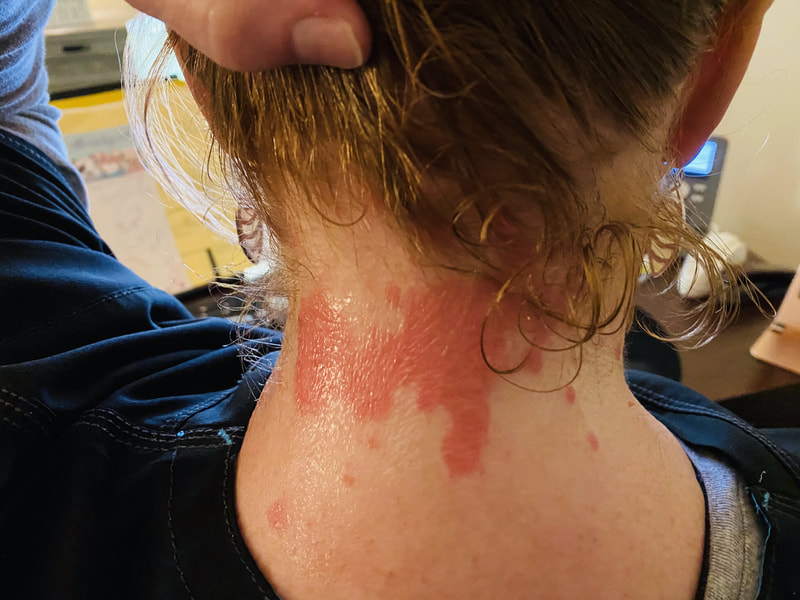
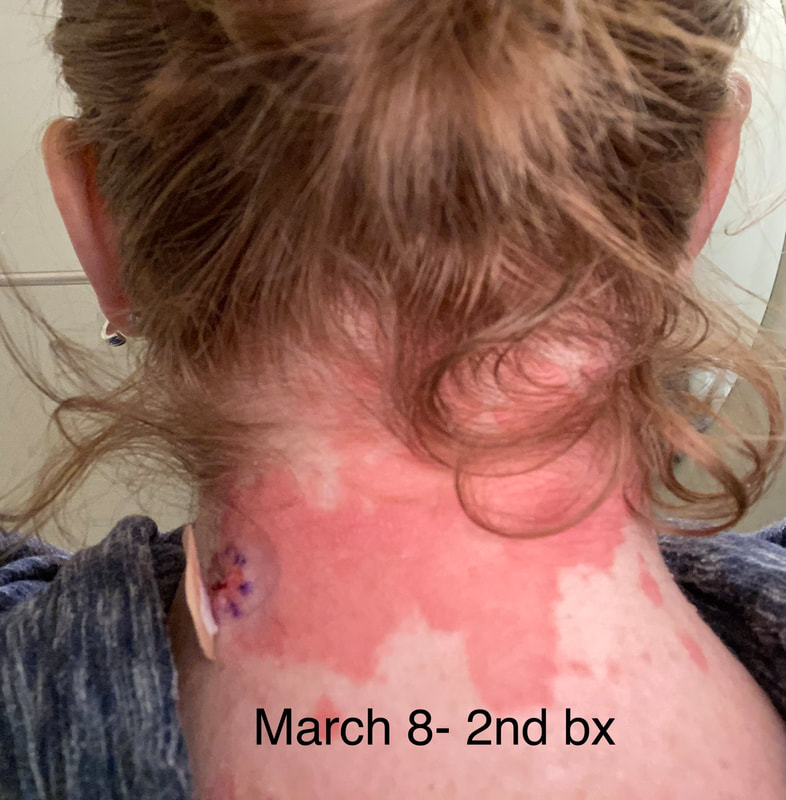
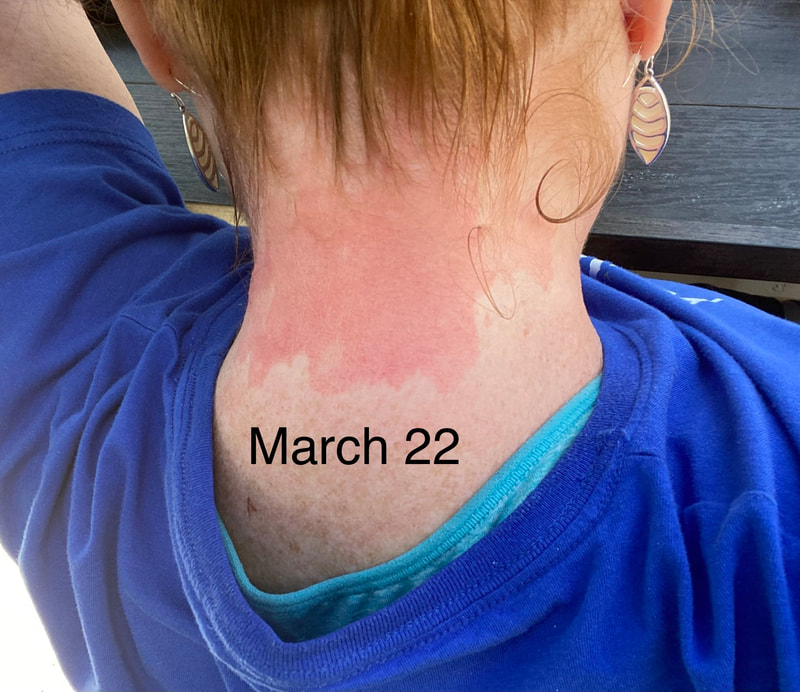
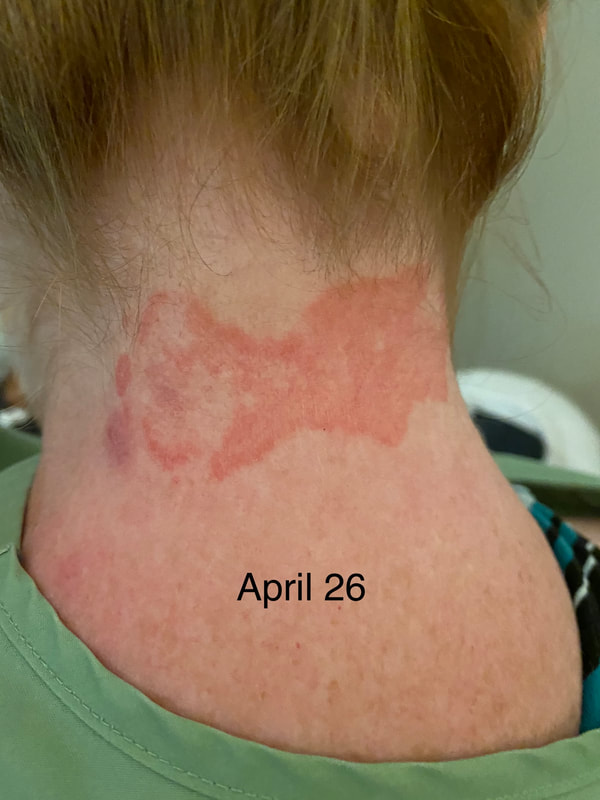
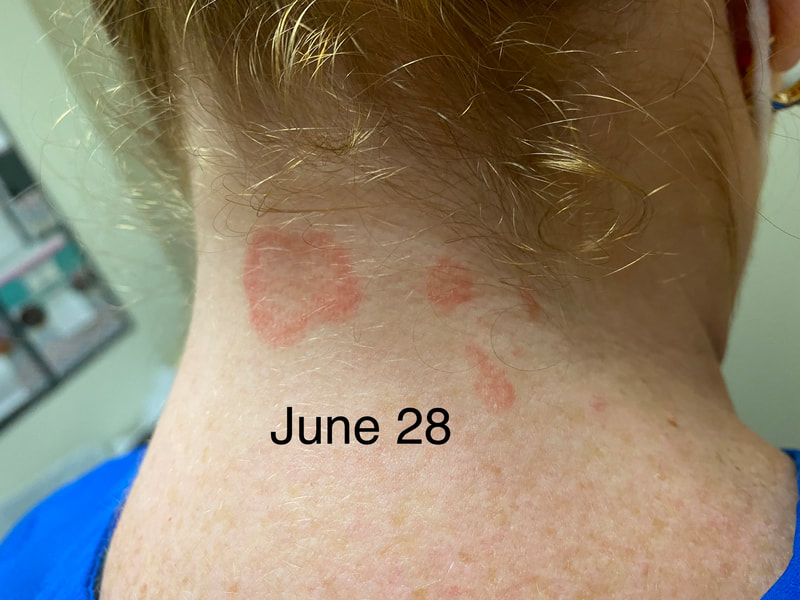
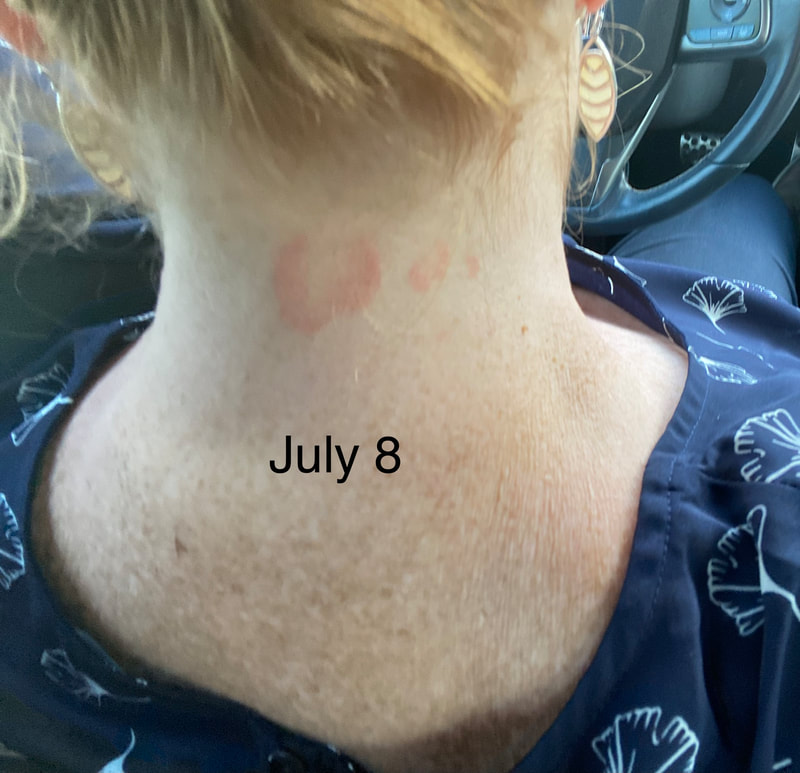
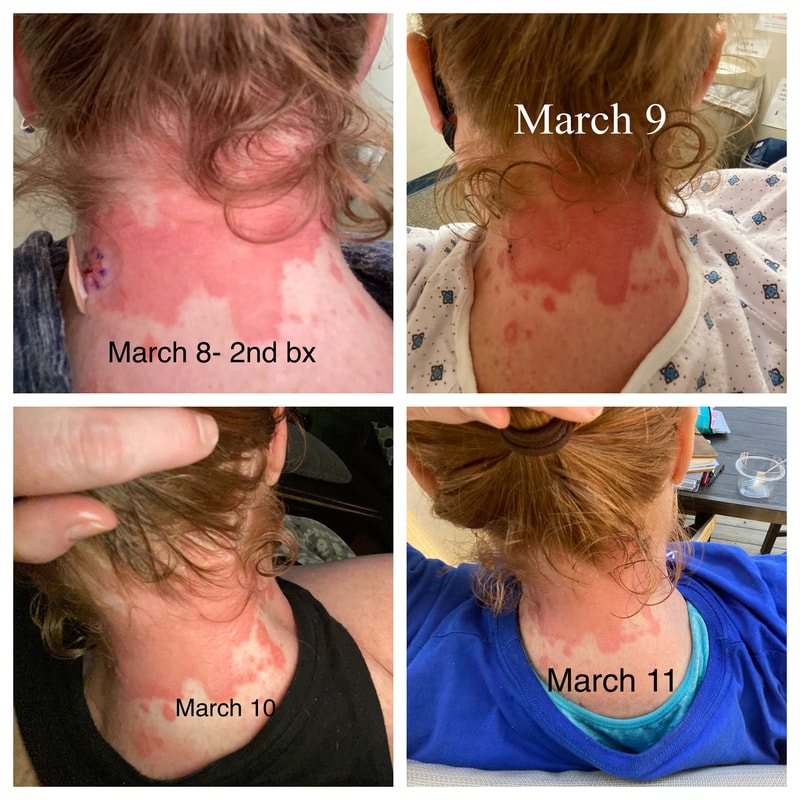
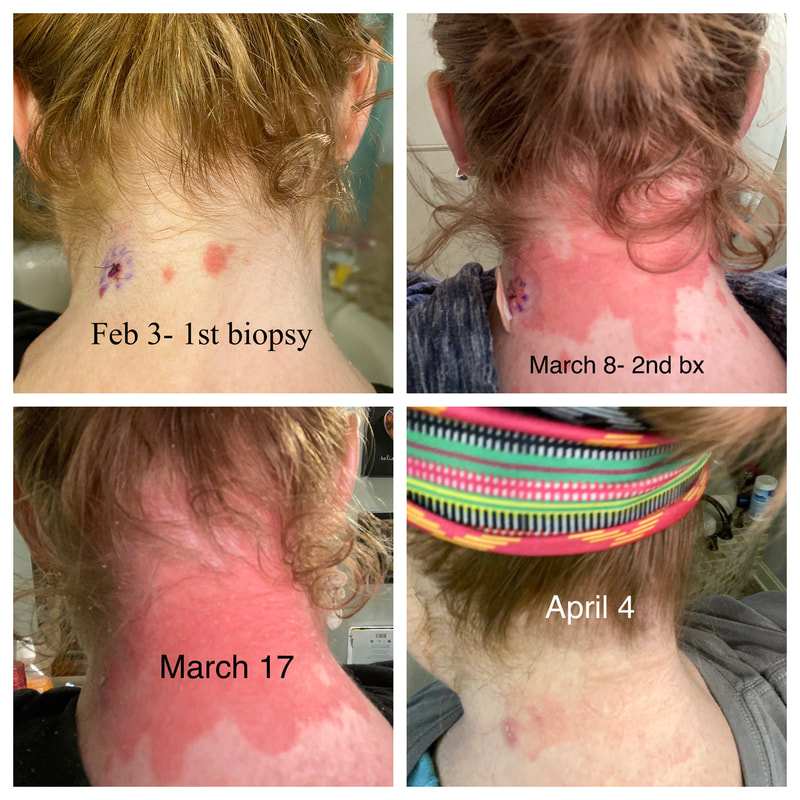
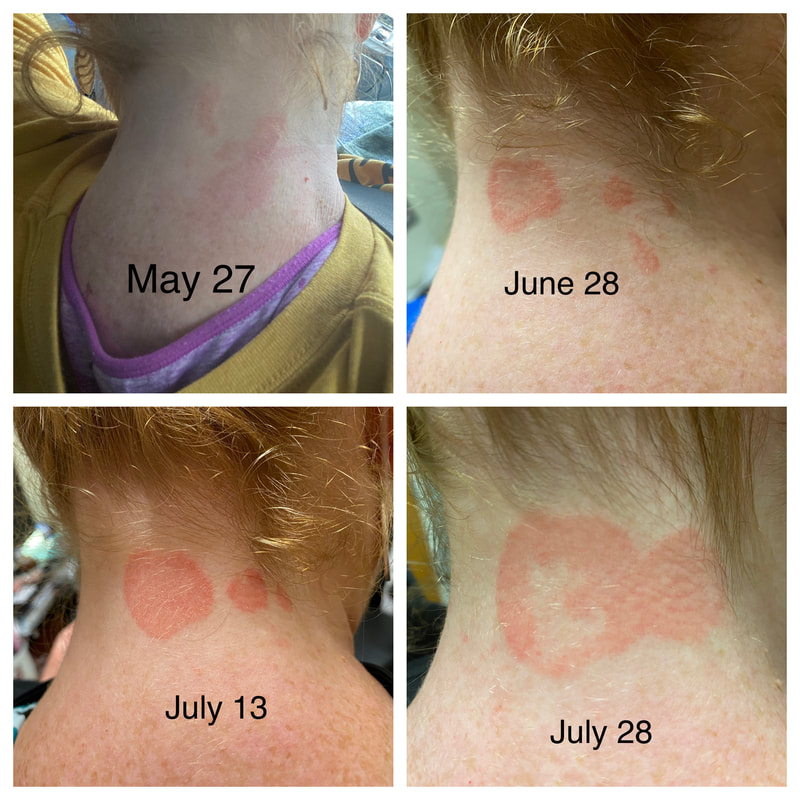
I hope this post has raised your awareness of sarcoidosis whether you are a patient, loved one, or healthcare professional. As I told a friend after she learned of my chronic illness, "My entire life changed after being diagnosed with sarcoidosis, but I didn't stop living." I hope this offers hope to anyone who is newly diagnosed or any sarcoidosis patient struggling right now. I see you. 💜 Jan 30, 2021- Feb 3, 2021 Red, painful eyes start with painful vision and light sensitivity (UVEITIS). Feb 3, 2020-Feb 8, 2020 Tiny dots of a rash begin on my neck- they don't itch, burn, or hurt at this point. I call my dermatologist to schedule a biopsy, assuming this must be related to my sarcoidosis. Feb 3-March 8, 2021 Rash kept getting bigger and more painful. Not responding to topical Rx creams. Went for 2nd biopsy on March 8th, the day I started my 30-day medical leave. Focused on walking, sleeping, hydrating, and eating clean. Also journaling and resting. March 8-April 8, 2021 Off work. Tried the AIP Diet. No gluten, no dairy, no sugar. Derm and Rheum also put heads together to double my Methotrexate dose. The diet was difficult but my joints and skin "felt" better even though my skin still needed lots of help! April 8- August 8, 2021 Back at work. Still working covid. Boys off for the summer during some of that time. Started Humira in May 2021 and stopped Methotrexate. Skin would wax and wane, but I would say it eventually cleared by early to mid-August. Joints feel much better on Humira. Energy level too. September 2021 Had my 2nd episode of uveitis. That responded quickly to Prednisone eye drops. Skin pretty clear, but under more stress with some work and family stuff. Delta variant of covid is ravaging my patient population and friends. Evidence of proteinuria again so will follow-up with my nephrologist (that's more sarc-related, less psoriasis-related). Still on Humira. Echo and PFT's slightly worse than last year, but lung & spleen CT's show that the Humira is controlling my sarcoidosis. March 2022 I have had at least 2 more episodes of uveitis since the last update. Skin stays mostly clear with the occasional flare in the anterior portion (front) of my neck. I wrote this piece for all of my fellow Psoriasis Warriors who are walking this painful, lonely road. It is SO HARD. One can think they are not a vain person, but when your LARGEST ORGAN (your skin) is literally on fire with inflammation, it's hard to "hide" from vanity, comparison, self-loathing, and frustration. If you love someone with psoriasis, please share this with them and with others who love them. I hope it brings someone comfort to know they are not alone and that there are those people who will love us no matter what. photo credit: Oluwaseyi Johnson Was it luck that the young mother of three bumped her head on the bed post and came in to see me? She was picking up a toy that had fallen into the abyss between the bed and the wall but I felt we better not miss an internal bleed in her brain those are rare but not good so I ordered the CT scan and we both went back to mothering our brood When the phone rang that night I can't remember if I dropped the phone It's a brain tumor, and it's big Can you call her at home? Was it luck when the car struck her from behind? Plastic and metal shredded and busted near the yellow line Her head hurt, her neck hurt to the doctor she went And the MRI that was supposed to check bones instead showed a hint of the cancerous tumor that was showing no signs it was in her thyroid, she had no symptoms God was definitely on time Was it luck when she came to tell me she was in pain? Her abdomen was cramping, her bowel movements had changed As the dutiful NP, I pulled up her old scans Has anyone ever mentioned your lungs to you ma'am? My lungs, why would they? My lungs are fine well it says on here that there's an issue - do you mind if I order a CT scan of them just to be safe? God was nudging me, directing me, showing me the way Pulmonary fibrosis? what in the world is that? Well, sweetheart, it's serious, sit down, we need to chat Unfortunately it's the same way my own disease often ends Here's my number, you can call me, I actually do understand Was it luck when she looked at me with frustration and contempt? Ma'am I'm sorry I just met you, let me see if I can help You can't help me she thought, they've already run all the tests God tapped my shoulder, I looked a little deeper, there was one thing left I'm sure it's nothing, but let's check this one last thing It's an ultrasound, I know you're frustrated, but let's do it, okay? Okay, she said, and I wasn't sure she would actually do it But days later the phone rang, there's an issue, there's fluid The young colleague who sent her to me called me for advice What do I order next? What do you think it is? I'm not sure what to try. So I made my suggestions and prayed I was wrong. Come on Lord, let's let this young patient just move along. But He couldn't and she couldn't and my colleague and I cried Another cancer, a bad one, it's not fair, it's not right Was it luck that I've found some of these things at the craziest times? Or was it God this whole time leading me with His light? I'm no saint, I'm a sinner, I get fired up, I have faults, I get loud But when I slow down and I pray and I look up to those clouds I can feel Him, sometimes it's so strong I just weep Like right now as I type this, and all those nights I've lost sleep These are a mere few of the miracles I have watched unfold in my tiny little town with my regular little folks Are we special? am I special? I don't claim any of it as mine It's His, I'm a vessel, I'm a sparrow, I'm a scribe Dear Lord, there have been so many times I have seen You. Why me? Am I doing it right? I sure do try, but I need You. When the going gets tough, and my stethoscope seems too much My alarm goes off again, and I feel Your gentle nudge You'll tell me when it's time. When my service is up. It wasn't luck, God. It's been You. Knowing that is enough. Amen. Author's note: Age and any identifying factors have been changed due to federal privacy laws. Please help support my fellow hope*writers by visiting their pieces using the prompt work LUCK:
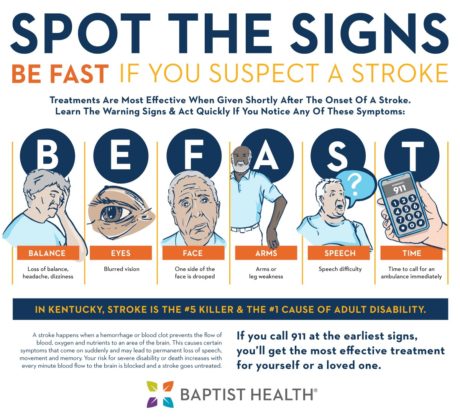
You are Not Lucky You are Blessed by Lisa Granger https://lisamarcelina.net/you-are-not-lucky-you-are-blessed/ Luck by Dianne Vielhuber https://simplewordsoffaith.com/wp-admin/post.php?post=10672&action=edit What Does Luck Have to Do With It? By Lori Shoaf https://www.lorishoaf.com/inspiringstories/what-does-luck-have-to-do-with-it Luck of an Evacuee by Ashley Olivine https://ashleyolivine.com/luck-of-an-evacuee/ In my 24 years of nursing / NP work, I have seen countless cardiac events either in action or the ramifications of such events. On a personal note, three of my four grandparents had strokes. I lost my paternal grandfather when I was only 4 and he was 55 due to a massive stroke. My paternal grandmother had stents in cardiac and non-cardiac arteries as well as "open heart surgery" CABG (coronary artery bypass graft). I have been affected by heart disease on a personal and a professional level, and I want to help patients understand the true risk of death and debility associated with cardiac events. Here are the top 10 reasons I refer patients to the cardiologist:
Let's talk a little more about each of these 10 conditions and how a patient may actually present to my office with these symptoms.
I have had patients in their thirties suffer from strokes and heart attacks. I have seen heart failure, cardiac arrhythmias, and high blood pressure in patients from childhood, young adulthood, and beyond. I doubt there is anyone in America who does not personally know someone who has been affected by heart disease. In honor of America's Go Red for Women Month (every February), I encourage you to schedule your wellness exam with your primary care provider and to start paying more attention to your heart rate, blood pressure, water intake, weight changes, and dietary choices. Your heart matters to me! Godspeed. How on earth is it already time for 2022? Where did 2021 go? I'm not sure, BUT, I am ready for 2022. 2021 was messy and ugly in many ways. On a personal level, it was unkind to my health. I received a new diagnosis of psoriasis in March and had to miss an entire month of work while my body was adjusting to new medications and my skin was trying to heal. October revealed an unexpected opportunistic infection (since I'm immunocompromised) that required strong antibiotics and made me feel pretty lousy. Since November 1, I have been hobbling around on painful swollen knees and am facing unexpected knee surgery. Pity party? Nah, not my style. Swallowing it all? That's my go-to. When I think about my health and how unfair it is that I've tried to take care of my body my whole life and I'm still getting the short end of the health stick, I can get pretty low. Then I think of all my patients who have it "worse." And I swallow it. I shove it down. I brush it off. But is that healthy? NOOOOOOOOOOOOOOOOOOO. So I'm learning to acknowledge my own feelings. I'm sad that my body is not behaving. I'm angry in some ways. I'm frustrated for sure. I'm still thankful that I can work for right now. I am beyond grateful for my parents who live 2 doors down and help me daily. I'm tired. I'm realizing I have X amount of energy each day and my family needs the bulk of it. If my job takes most of it then I'm robbing my family of my best self. Filing for disability has been on my mind more in the past 9 months than it ever has during this 5 year sarcoidosis journey. So what next? New year, new adventures, new planner, new goals, new.... what else is new now that I'm 45? I have a lot of old. Old hurts. Old unmet needs. Old furniture. Old clothes. Old shame. Old junk in my kitchen drawers. Old relationship issues that deserve a conversation. An old van that has chipping paint but it's paid for and gets us to ball tournaments. I think the reflex for all of us is to replace the old with the new and that will make it all better. New clothes. The newest kitchen gadget. New furniture or decor, ON TREND, my dear! A shiny new SUV that costs more than most people's annual salary and gets 12 mpg. But boy does it look good and that's what counts, right? I'm no longer trying to replace the old just by reflex. It's harder to keep it and try to keep it running. Purging the clothes and kids' toys is definitely good, but when we throw out things that still work but aren't "good enough" for whatever standards, what does that say about us? Who and what have you thrown away and replaced with newer and easier? (ouch)... I'm falling apart health-wise in a lot of ways, but I "still work." Will my family or employer throw me out? Will my friends forget about me if I'm not as active and fun as I used to be? Where does that leave me? As an Enneagram 3 (Performer, Success Driven), I've been gut-punched this year by my body's betrayal. But God must be telling me something. I know He has a plan. I have to trust and slow down and just be. NOT. MY. STRONG. SUIT. Perhaps 2021 leaves you feeling like I do. Maybe you lost someone you loved. Maybe you were also betrayed by either your body or someone you trusted. Maybe you felt out of control all year like I did? Maybe you spent too many hours googling vaccines and viruses and death tolls like most of the world. Maybe you feel all the "junk" you've shoved down and swallowed for however long starting to surface and want to be named and noticed. I feel that with you. 2022 can be a renewal for us, my friends. I'm going to intentionally name what's working, what's not working, what is worth repair, and what really needs to be purged from my life. This goes for relationships, time spent, health choices, what I consume digitally and physically, items in my home and closet, and my thought life. I'm going to check myself when I just want to replace the old for that quick dopamine hit. I'm going to try to sit in the uncomfortable and define what's causing it. I can't keep running 90 mph. 2022 is for slowing down. It is for evaluation. It is for growing up, finally. Godspeed. I do want you to listen to the podcast, because I think there are some big pearls in this interview, but here are a few highlights:
Find out who is in your circle:
Plan as much as you can ahead of time:
Final pro tips: -Keep a medical binder of all your paperwork -Have a designated inbox for all incoming papers (follow The Planning Woman for more on this) -Apply for intermittent FMLA with your employer -My personal pro tip: PET THERAPY! 🐶🐱 Charlie the Dachshund makes everything better!
When a patient presents with hair loss, I obtain a thorough history:
I then perform a thorough physical exam and order the following tests:
That may not “answer” your question but I hope it helps you know what a clinician will be looking for with this presentation of hair loss. 🩺👩⚕️ Personally, I have dealt with hair loss from taking Methotrexate for my sarcoidosis.
It started coming out in clumps in the shower and then in my brush. I soon had very patchy areas of hair loss all over my scalp. My hairdresser advised me to stop applying heat to my hair when possible, to wash my hair less frequently, to avoid ponytail holders when possible, and to avoid any hair color or harsh chemicals. I usually got some blonde highlights in the spring put in my naturally red hair, but I went without those for 4 years while I was on Methotrexate. My rheumatologist increased my Folic Acid dose from 1 mg to 2 mg daily, and I ordered Biotin off Amazon Subscribe and Save. I took the Biotin daily to help with hair growth. I am finally off Methotrexate and on Humira and am seeing hair growth again. Losing my hair was very emotional for me. My bright red hair has defined me for so long. I now knew what all of my patients struggling with hair loss from chemo or other medical reasons were feeling, and boy was it a wake up call. My heart goes out to anyone struggling with hair loss. Much love to you and I hope this helps. Throughout my career, I have had to deliver hard news to my patients. I have had to deliver even worse news to their families. It is the LEAST favorite part of my job, but I have found some comfort knowing I am delivering the news with compassion and empathy. I usually know the patient and family very well, and I think that means a lot. These suggestions may be helpful when faced with a difficult diagnosis.
Let's look at each suggestion in detail:
I am in a unique position in that I have both delivered and received hard news. At the age of 40, when my youngest son was 4, I was told I probably have lymphoma AND multiple sclerosis over the phone by a nurse. I was told to get an appointment with an oncologist and a neurologist as soon as possible. Many blood tests, imaging tests, and biopsies later, I was finally told that "you don't have cancer! And I don't think you have MS but I'm not sure. What you do have is a lifelong incurable autoimmune disease that can attack any organ and can be difficult to treat. And by the way, nobody has really heard of it and even us doctors have to google it when we see it on a chart."
So maybe those weren't his exact words, but it was close. And there will be a lot more to that story to come in my posts. I wish someone had used tip #3 with me when delivering my news. Here are 10 easy ways to support someone with a chronic illness:
I have been living with a chronic illness for 5 years now. My family and friends have been a huge source of support. Even as they've tried to love me, I've witnessed their looks of "what can I do?" or "what should I say?". Most chronic illnesses are unique and involve multiple appointments with various specialists, countless medications, and years of simply managing one's health. These concrete examples can really help your loved one and make them feel important.
How to have an effective office visit with your provider: There are some tried and true ways to have a productive, meaningful visit with your medical provider. As a patient with a chronic illness AND a family nurse practitioner, I have the inside track.
If you need more frequent office visits, ask for them. Your provider is PAID to see you. Your insurance is billed for those visits where as most providers do not bill for phone calls or portal messages. If you end up needing them before your designated 3 or 6 month follow-up and you have more than 1-2 simple questions, PLEASE schedule an office visit. As a provider with complicated patients of my own, I would much rather have that patient in the office with me to have a discussion than to do multiple back-and-forths over the portal. It’s better patient care. AND my time is used wisely in my employer’s mindset. Medicine is a business. Although so many of us really do care!!!  What do we say when we don't know what to say? We have all been there. Someone dies unexpectedly. Someone receives a terrible diagnosis. A divorce comes out of nowhere. A tragic accident. Our partner says something cruel or doesn't meet our emotional needs. A friend is struggling with infertility or has a miscarriage. Our friend is venting about a difficult situation. Here are some tips for what to say and what not to say: Do / say this:
Don't do / say this:
CHECK OUT THE BOOK "I HEAR YOU" BY MICHAEL SORENSON FOR AN IN-DEPTH DISCUSSION ON ACTIVE AND EFFECTIVE LISTENING. WORTH THE READ!
|
Proudly powered by Weebly